Fatty Liver Symptoms: 10 Warning Signs, Diet Chart & How to Reverse It Naturally

⚡ Quick Summary
You're feeling tired all the time, your abdomen feels heavier than usual, and then one day your blood report casually mentions "fatty liver." For many women, this is how the journey begins — subtle symptoms that don't seem alarming at first, but gradually start affecting energy, digestion, and overall well-being.
The truth is, fatty liver disease is often ignored until it becomes more serious. In most cases, the body starts sending early warning signs long before the condition progresses. But because these symptoms — fatigue, bloating, mild weight gain — are vague, they're easily brushed off as stress, hormonal changes, or a busy lifestyle.
In this guide, we'll break down 10 common fatty liver warning signs, explain why women face a higher risk due to hormonal and metabolic factors, and show you how to reverse fatty liver naturally with the right nutrition and lifestyle strategies.
What Is Fatty Liver Disease (NAFLD)?
Fatty liver, medically known as hepatic steatosis, refers to a condition where excess fat accumulates within liver cells — typically when more than 5% of the liver's weight is made up of fat. While a small amount of fat in the liver is normal, excessive buildup interferes with its function over time.
There are two main types. Non-alcoholic fatty liver disease (NAFLD) occurs in individuals who consume little to no alcohol and is largely driven by metabolic factors such as insulin resistance, poor diet, and sedentary lifestyle. Alcoholic fatty liver disease (AFLD) is caused by excessive alcohol intake. Today, NAFLD is far more common and is increasingly being seen even in younger individuals and those who appear outwardly healthy.
In the Indian context, fatty liver has become a silent epidemic. Studies suggest that nearly 30–40% of Indian adults may have some degree of fatty liver disease. What makes it particularly concerning is that it often develops without obvious symptoms in the early stages.
Fatty liver is not just a liver condition — it is deeply connected to overall metabolic health. It is often a manifestation of underlying insulin resistance, high triglycerides, abdominal obesity, and chronic inflammation. This is why addressing fatty liver requires a broader metabolic approach rather than focusing on the liver in isolation.
Fatty liver is a sign of deeper metabolic dysfunction. Understanding the full picture of your metabolic health — including blood sugar, insulin resistance, and inflammation — is the foundation for reversing it effectively.
The Complete Guide to Metabolic Health: Causes, Symptoms & Reversal →10 Fatty Liver Symptoms You Should Not Ignore
Fatty liver is often called a "silent" condition because many people don't experience obvious symptoms in the early stages. However, the body usually gives subtle signals that something isn't right — you just need to know what to look for.
Persistent Fatigue and Low Energy
One of the most common early signs — feeling tired even after adequate sleep. The liver plays a key role in energy metabolism, and when it's overloaded with fat, energy production becomes less efficient. This type of fatigue doesn't improve with rest.
Dull Discomfort or Heaviness in the Upper Right Abdomen
You may notice a dull ache or persistent heaviness in the upper right side of your abdomen — where the liver is located. It's not always painful, but can feel like a constant fullness or pressure in that area.
Unexplained Weight Gain — Especially Around the Belly
Unexplained weight gain, particularly abdominal fat accumulation, is a strong indicator of underlying metabolic dysfunction closely linked to fatty liver. If your waist is expanding despite no major change in diet, this is worth investigating.
Signs of Insulin Resistance
Frequent sugar cravings, energy crashes after meals, brain fog after eating carbohydrates, or difficulty losing weight despite efforts are all signs of insulin resistance — the primary driver of fatty liver disease. These symptoms often precede elevated liver enzymes on blood tests.
Elevated Liver Enzymes (ALT and AST) on Blood Tests
In many cases, fatty liver is first detected through blood tests showing elevated liver enzymes (ALT and AST), even when there are no visible symptoms. This is why routine blood work is so important — particularly if you have metabolic risk factors.
Dark, Velvety Skin Patches (Acanthosis Nigricans)
Dark, velvety skin patches around the neck, armpits, or knuckles — a condition known as acanthosis nigricans — are strongly associated with insulin resistance. This is one of the most visible external signs that metabolic dysfunction and potential fatty liver may be present.
Bloating and Digestive Discomfort After Meals
Persistent bloating after meals, a feeling of heaviness in the stomach, or slow digestion can indicate that the liver and gut are not functioning optimally. The gut-liver axis is closely linked — poor liver health often manifests as digestive symptoms.
Loss of Appetite or Disinterest in Food
As fatty liver progresses, some people experience a general loss of appetite or reduced interest in food. This is the liver signalling that something is wrong with its metabolic processing capacity.
Jaundice — Yellowing of Skin and Eyes
In more advanced stages, jaundice may develop — a visible yellowing of the skin and whites of the eyes. This indicates significant liver stress and impaired bilirubin processing. Jaundice warrants immediate medical attention and investigation.
Confusion or Difficulty Concentrating (Hepatic Encephalopathy)
In severe cases, when liver function is significantly compromised, individuals may experience confusion, forgetfulness, or difficulty concentrating — a condition known as hepatic encephalopathy. This is a late-stage sign that requires urgent medical assessment.
Fatty Liver Symptoms in Women: Why Are Females at Higher Risk?
While fatty liver disease can affect both men and women, certain hormonal and life-stage factors make women particularly vulnerable. In clinical practice, it's very common to see women experiencing symptoms like fatigue, weight gain, and mood changes without realising these could be linked to underlying liver and metabolic dysfunction.
Estrogen decline at menopause
During the reproductive years, estrogen offers some protective effect on metabolism and fat distribution. However, during menopause, as estrogen levels decline, there is a noticeable shift toward increased visceral fat accumulation — particularly around the abdomen. This type of fat is closely linked to insulin resistance and fatty liver development.
PCOS and insulin resistance
Conditions like PCOS (Polycystic Ovary Syndrome) significantly increase the risk. Studies suggest that nearly 50–70% of women with PCOS may have fatty liver, largely due to underlying insulin resistance. Symptoms like stubborn weight gain, irregular cycles, acne, and fatigue often overlap with metabolic dysfunction, making fatty liver easy to miss unless specifically screened for. For more on managing PCOS with nutrition, read our PCOS Diet Plan →
Pregnancy and gestational risk
Women with insulin resistance or undiagnosed fatty liver are at higher risk of developing gestational diabetes, which not only affects pregnancy outcomes but also increases the long-term risk of metabolic disorders.
What makes this more challenging is that many symptoms of fatty liver in women — chronic fatigue, difficulty losing weight, bloating, and mood fluctuations — are often attributed to stress, hormonal imbalance, or lifestyle factors. This overlap frequently delays diagnosis and intervention.
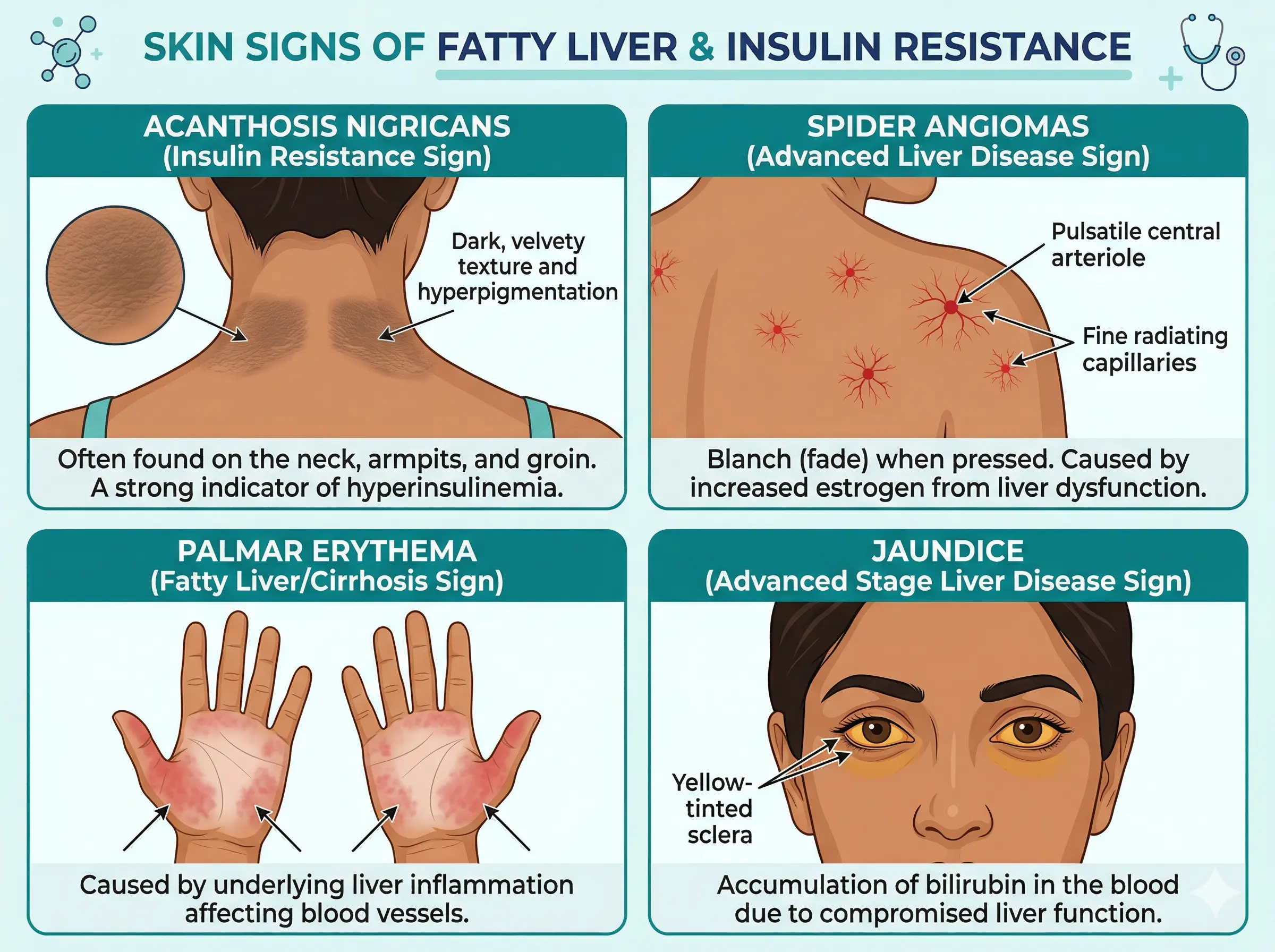
Fatty Liver Symptoms on the Face and Skin
Your skin often reflects what's happening internally, and in many cases, fatty liver and insulin resistance can show up through visible changes before they're detected on a report. Here are the key skin signs to watch for:
| Skin Sign | What It Looks Like | What It Signals |
|---|---|---|
| Acanthosis Nigricans | Dark, velvety patches — neck, underarms, knuckles | Insulin resistance (primary driver of fatty liver) |
| Spider Angiomas | Tiny red, spider-like blood vessels on face, neck, or chest | Underlying liver stress or portal hypertension |
| Palmar Erythema | Unusual redness of the palms | Liver dysfunction affecting blood vessel dilation |
| Unexplained Itching | Persistent itching without visible rash | Bile acid buildup when liver function is impaired |
| Jaundice | Yellowish tint in skin and whites of the eyes | Significant liver dysfunction — requires urgent evaluation |
What Causes Fatty Liver Disease?
Fatty liver disease rarely results from a single cause — it develops when multiple metabolic and lifestyle imbalances accumulate over time. Here are the key contributing factors:
| Cause | How It Contributes | Significance |
|---|---|---|
| Insulin Resistance | Excess glucose is converted into fat and stored in the liver | Primary driver |
| High Refined Carbs and Sugar | Constant blood sugar spikes drive liver fat accumulation — especially fructose | Major contributor |
| Obesity and Visceral Belly Fat | Visceral fat releases inflammatory chemicals that worsen insulin resistance | Major contributor |
| Metabolic Syndrome | Cluster of high blood sugar, high triglycerides, low HDL, and large waist | Closely linked |
| Sedentary Lifestyle | Reduces the body's ability to burn glucose and fat for energy | Significant |
| Hormonal Imbalances | PCOS, hypothyroidism, menopause promote abdominal fat storage | Important in women |
| Rapid Weight Loss | Floods the liver with fat as it is broken down too quickly | Often overlooked |
| Nutrient Deficiencies | Low choline, vitamin B12, vitamin D, and omega-3 impair fat metabolism | Correctable |
| Genetic Predisposition | Gene variants (PNPLA3, TM6SF2) increase susceptibility in South Asians | Identifiable via DNA test |
Genetic Risk Factors for NAFLD: Why Some People Are More Susceptible
Two individuals may eat similar diets and have similar body weight, yet one develops significant fat accumulation in the liver while the other does not. A significant part of this difference is explained by genetic variations that influence how the liver processes fat and regulates inflammation — particularly relevant for South Asian populations.
PNPLA3 Gene (I148M Variant): The Strongest Genetic Predictor
The PNPLA3 (I148M variant) is considered the strongest genetic predictor of NAFLD identified so far. People carrying this variant have reduced efficiency in breaking down stored fats in the liver, leading to triglyceride accumulation even when other metabolic risk factors are relatively mild. This variant is more prevalent in South Asians, which partly explains why fatty liver disease often appears at lower body weights and younger ages in the Indian population.
TM6SF2: Regulating Liver Fat Export
Certain variants in TM6SF2 reduce the liver's efficiency in packaging and exporting triglycerides into the bloodstream. When this export process is impaired, fat accumulates inside liver cells. Interestingly, these individuals may show normal or low cholesterol levels on blood tests — even while liver fat continues to accumulate internally.
MBOAT7: Linking Fat Accumulation and Inflammation
Variants in MBOAT7 are associated with increased susceptibility to liver inflammation and fibrosis. While PNPLA3 and TM6SF2 influence fat accumulation, MBOAT7 influences how the liver responds to that fat — making it particularly relevant for assessing long-term disease progression risk.
For individuals with PNPLA3 risk variants, reducing refined carbohydrates and fructose has a disproportionately large benefit. DNA testing can identify these gene variants and help create a targeted nutrition plan for your specific metabolic profile.
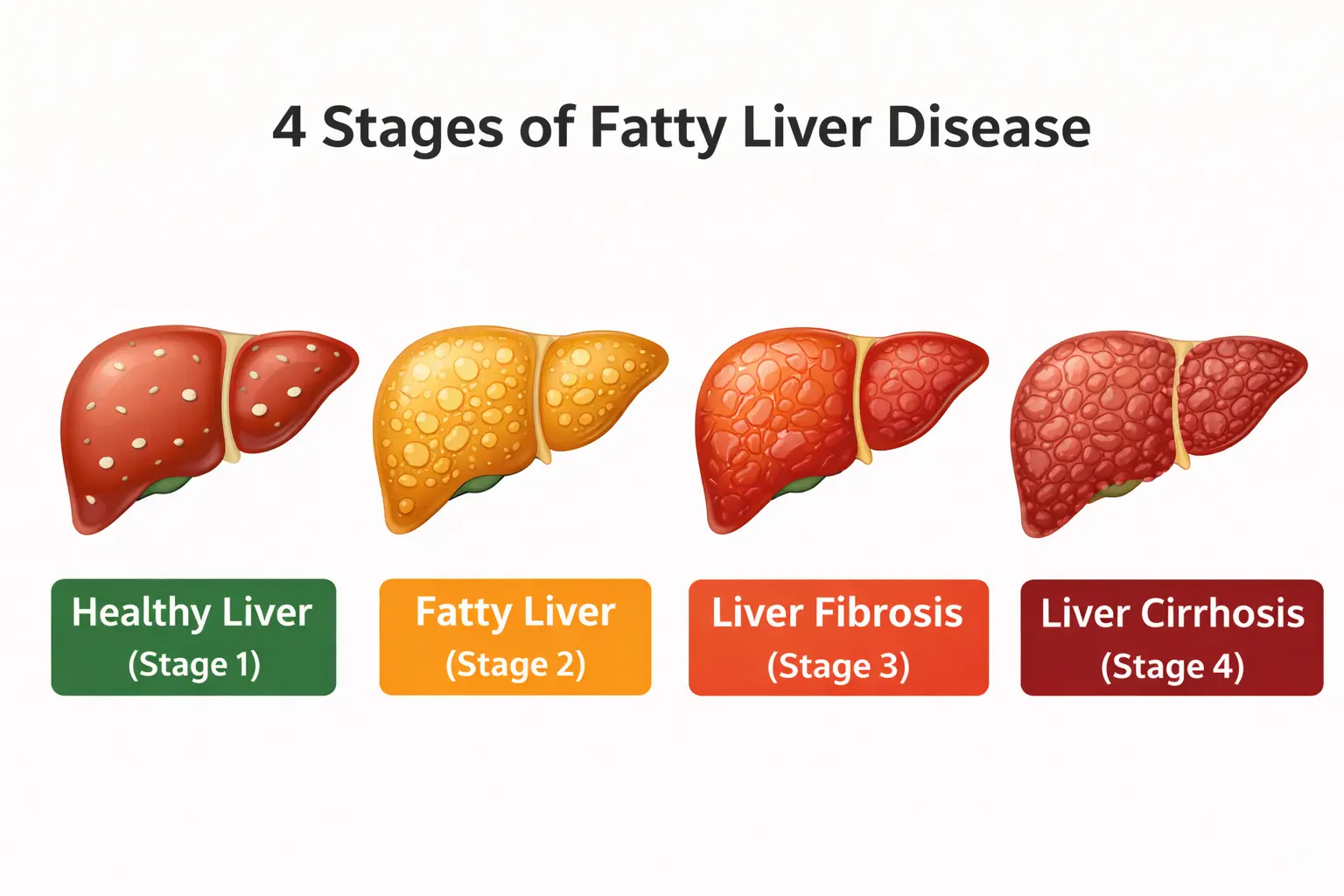
How DNA and Nutrigenomics Influence Metabolic Health →4 Stages of Fatty Liver Disease — and What They Mean for You
Fatty liver is not a single-stage condition — it progresses gradually if left unaddressed. Understanding these stages helps you know where you stand and how urgently you need to act.
Simple Fatty Liver (Steatosis)
Fat accumulates in liver cells but there is no inflammation or damage yet. Most people have no symptoms at this stage and it is often detected incidentally. Completely reversible with nutrition and lifestyle changes.
NASH (Non-Alcoholic Steatohepatitis)
Fat accumulation is accompanied by inflammation and mild liver cell damage. Some people begin to experience fatigue or abdominal discomfort. Still largely reversible with early intervention.
Fibrosis (Scar Tissue Formation)
Ongoing inflammation leads to scar tissue in the liver. The liver still functions, but its efficiency declines. Reversal becomes more challenging but is often partially possible with consistent medical and lifestyle support.
Cirrhosis (Advanced Scarring)
Extensive scarring severely affects liver function. Generally irreversible, but progression can be slowed or halted with treatment and lifestyle changes. Requires specialist medical management.
How to Diagnose Fatty Liver: Tests to Ask Your Doctor For
| Test | What It Measures | Notes |
|---|---|---|
| ALT and AST (Blood Test) | Liver enzyme levels — elevated values indicate liver stress | Fatty liver can be present even when values are normal in early stages |
| Abdominal Ultrasound | Visualises fat accumulation in the liver | Most common first-line screening; non-invasive and widely available |
| FibroScan | Measures liver stiffness (fibrosis) and fat content non-invasively | Best for staging and tracking progress over time |
| MRI / CT Scan | Detailed imaging of liver structure and fat distribution | Used when ultrasound is inconclusive or more detail is needed |
| Liver Biopsy | Gold standard for confirming NASH and fibrosis staging | Invasive — only used when non-invasive tests are inconclusive |
| Lipid Profile + HbA1c | Triglycerides, HDL cholesterol, blood sugar control | High triglycerides and low HDL are strongly associated with NAFLD |

Which blood tests actually reveal metabolic dysfunction? Beyond liver enzymes, there are key markers that paint a much clearer picture of your metabolic health and liver risk.
11 Blood Tests That Reveal Your True Metabolic Health →Is Your Fatty Liver Linked to Your Genes?
Some people develop fatty liver even at normal weight. Others have a diet that seems fine, yet liver fat accumulates. Your genetic profile — including PNPLA3 and other metabolic genes — determines how your body processes fat. Find out your metabolic type in 3 minutes.
Take the Free Metabolic Quiz →No signup required · 3-minute quiz · Instant results
Fatty Liver Diet: What to Eat and What to Avoid
When it comes to reversing fatty liver, diet is the single most powerful tool available. The goal is to reduce liver fat, improve insulin sensitivity, lower inflammation, and support the liver's natural fat metabolism and export mechanisms.
The most important principle is this: it's not about following a strict or complicated diet. It's about consistently replacing the foods that drive fat accumulation with foods that support liver healing. A gradual, sustainable approach works far better than extreme dietary restrictions.
Foods to Eat for Fatty Liver Reversal
| Food Category | ✅ Eat Freely | ❌ Avoid or Limit |
|---|---|---|
| Grains | Oats, bajra, jowar, ragi, brown rice, quinoa, multigrain roti | White rice (excess), maida, white bread, naan, bakery products, biscuits |
| Proteins | Dal, moong, legumes, eggs (choline source), grilled fish, chicken, tofu, paneer (limited) | Processed meats, sausages, salami, fried meat, nuggets |
| Fats and Oils | Olive oil, cold-pressed oils, walnuts, flaxseeds, chia seeds, fatty fish (omega-3) | Vanaspati, dalda, excess butter, cream, excess saturated fat |
| Vegetables | Leafy greens (spinach, methi), broccoli, cauliflower, beetroot, garlic, all non-starchy vegetables | Deep-fried vegetables in any form |
| Fruits | Berries, apple, papaya, guava (low glycaemic, high fibre) | Packaged fruit juices, sugary fruit, large portions of high-sugar fruits |
| Beverages | Green tea (antioxidant support), lemon water, plain water, buttermilk | Sodas, energy drinks, packaged juices (high fructose), alcohol (completely) |
| Herbs & Spices | Turmeric, ginger, garlic — all support liver detox and reduce inflammation | Excess salt, high-sodium condiments and pickles |
| Sweeteners | Small amounts of natural honey or jaggery if needed | Sugar, refined sweeteners, artificial sweeteners (disrupt gut-insulin axis) |

7-Day Indian Diet Chart for Fatty Liver
This meal plan focuses on stable blood sugar, adequate protein, high fibre, and anti-inflammatory foods — the four pillars of fatty liver reversal through diet. Portion sizes should be appropriate to your individual requirements.
How to Reverse Fatty Liver Naturally: 6 Evidence-Based Strategies
The encouraging truth about fatty liver disease is that it is largely reversible — especially in Stages 1 and 2. The focus should be on addressing the root metabolic causes rather than looking for quick fixes. Here are the six most important strategies:
Achieve 5–10% Weight Loss
Even modest weight loss significantly reduces liver fat, improves insulin sensitivity, and lowers inflammation. Aim for gradual, sustainable loss — not crash dieting.
Exercise Regularly (150 Min/Week)
Brisk walking, cycling, or strength training all improve insulin sensitivity and support fat metabolism. Exercise is one of the most effective single interventions for NAFLD.
Prioritise Sleep (7–8 Hours)
Poor sleep raises cortisol, worsens insulin resistance, and slows liver recovery. Consistent, restful sleep is non-negotiable for metabolic healing.
Manage Stress Effectively
Chronic stress elevates cortisol, promoting visceral fat storage and worsening metabolic imbalance. Yoga, breathing exercises, and mindful routines all help regulate the stress response.
Avoid Alcohol Completely
Even in NAFLD (non-alcoholic), alcohol adds additional stress on the liver and significantly delays recovery. Complete avoidance is strongly recommended during the reversal phase.
Targeted Supplement Support
Omega-3 fatty acids, vitamin E, vitamin D, milk thistle, berberine, and probiotics may all support liver health. Use under professional guidance based on your individual needs and blood markers.
Can Fatty Liver Be Reversed? What the Evidence Shows
The most encouraging part about fatty liver disease is straightforward: yes, it can be reversed — particularly when identified early. In Stage 1 (simple fatty liver) and Stage 2 (NASH), the condition is fully reversible with the right combination of nutrition, lifestyle changes, and metabolic correction.
With consistent efforts, many people start seeing measurable improvements within 3–6 months. Research and clinical practice both confirm that even a 5–10% reduction in body weight can significantly reduce liver fat, improve liver enzyme levels, and enhance overall metabolic health. In some cases, 10% weight loss can almost completely eliminate excess fat from the liver.
The key word, however, is consistency. Quick fixes or short-term diets may give temporary results, but sustainable changes in eating patterns, physical activity, sleep, and stress management are what drive long-term reversal. And if left untreated, fatty liver can gradually progress to fibrosis or cirrhosis — which is why ignoring early signs or delaying action has real long-term consequences.
Fatty Liver and Related Metabolic Conditions
Fatty liver rarely exists in isolation. It is closely connected with other metabolic and hormonal disorders and is best understood as part of a larger metabolic network where multiple conditions influence each other.
| Related Condition | How It Connects to Fatty Liver |
|---|---|
| Type 2 Diabetes and Insulin Resistance | Bidirectional relationship: insulin resistance causes liver fat accumulation, and fatty liver worsens insulin sensitivity. Both conditions feed into each other if not addressed together. Read more: Insulin Resistance Guide → |
| PCOS | 50–70% of women with PCOS may have fatty liver due to underlying insulin resistance. Symptoms overlap significantly — weight gain, irregular cycles, fatigue, and metabolic dysfunction coexist. |
| High Cholesterol and Triglycerides | Elevated triglycerides and low HDL are strongly associated with fatty liver. The liver's impaired fat export contributes to abnormal lipid profiles in the bloodstream. |
| Hypothyroidism | A sluggish thyroid slows metabolism, promotes weight gain, and worsens lipid imbalances — all of which increase liver fat accumulation. |
| Cardiovascular Disease | Elevated triglycerides, chronic inflammation, and insulin resistance associated with fatty liver directly contribute to plaque formation and vascular damage. |
High cholesterol and fatty liver frequently coexist. If your blood tests show elevated triglycerides or low HDL alongside fatty liver findings, both conditions need to be addressed together through diet.
Indian Diet Chart for High Cholesterol: 7-Day Meal Plan →Final Takeaway
Fatty liver disease is extremely common, often silent, but highly reversible — especially when identified early. The challenge is that most people ignore the early warning signs or discover it only through routine tests. By the time symptoms become obvious, the condition may have already progressed. That's why early detection and timely action are crucial.
The good news is that reversal does not require extreme measures. Consistent changes in diet, regular exercise, better sleep, and stress management can significantly reduce liver fat and improve overall metabolic health. However, what works best is not a one-size-fits-all approach. Personalisation matters — your nutrition, lifestyle, and even genetic makeup all influence how your body responds and heals.
If you want to take a more targeted approach, unlock.fit combines DNA insights, blood markers, and lifestyle analysis to create a personalised plan tailored to your body and goals.
Frequently Asked Questions
Yes, in most cases — especially in Stage 1 (simple fatty liver) and Stage 2 (NASH) — fatty liver can be completely reversed with the right diet, lifestyle changes, and metabolic correction. Research shows that even a 5–10% reduction in body weight can significantly reduce liver fat and normalise liver enzyme levels. The key is consistency over several months, not a quick fix.
With consistent efforts, measurable improvements are typically seen within 3–6 months. Liver enzyme levels (ALT, AST) may normalise within 8–12 weeks of dietary changes. Structural reduction of liver fat takes longer. The timeline depends on the severity of the condition and how consistently lifestyle changes are followed — consistency matters far more than intensity.
In the early stages, fatty liver may not cause major issues. However, if left untreated, it can progress to non-alcoholic steatohepatitis (NASH), fibrosis, and in advanced cases, cirrhosis — which is largely irreversible. It also significantly increases the risk of type 2 diabetes, cardiovascular disease, and in rare cases, liver cancer. This is precisely why early detection and intervention are so important.
No. Even in non-alcoholic fatty liver disease (NAFLD), alcohol adds significant stress on the liver and slows down recovery substantially. Complete avoidance is strongly recommended — especially during the reversal phase. Even occasional drinking can disrupt the healing process.
Commonly used supplements include omega-3 fatty acids (reduce liver inflammation and improve lipid profile), vitamin E (antioxidant support for liver cells), vitamin D (metabolic and immune function), milk thistle (supports liver detox pathways), berberine (improves insulin sensitivity), and probiotics (support the gut-liver axis). These should always be taken under professional guidance based on individual blood markers and needs.
Fatty liver itself does not directly cause weight gain, but it is strongly linked to insulin resistance and metabolic dysfunction, which make weight gain — especially around the abdomen — significantly more likely. The relationship is bidirectional: excess abdominal fat worsens fatty liver, and fatty liver worsens insulin resistance. Breaking this cycle requires addressing both simultaneously.
There is a significant genetic component. Gene variants such as PNPLA3 (I148M), TM6SF2, and MBOAT7 have been strongly linked to higher susceptibility to NAFLD, and are more prevalent in South Asian populations. This partly explains why fatty liver often develops at lower body weights and younger ages in Indians compared to other populations. However, lifestyle and dietary habits remain the most important and modifiable factors.
Skin signs of fatty liver and related insulin resistance include dark, velvety patches around the neck, underarms, or knuckles (acanthosis nigricans), tiny red spider-like vessels on the face or chest (spider angiomas), unusual redness of the palms (palmar erythema), unexplained itching without a visible rash, and in advanced stages, jaundice — a yellowing of the skin and whites of the eyes. These skin changes can appear before the condition is detected on blood tests.
Yes. DNA testing can identify gene variants like PNPLA3 that affect how your liver processes fat and responds to specific dietary inputs — particularly refined carbohydrates and fructose. This helps create a more targeted nutrition plan. For example, individuals with the PNPLA3 I148M variant benefit most from reducing refined carbohydrates and fructose specifically, rather than just following a generic low-fat diet.
Free Consultation · Limited Slots
Ready to Reverse Your Fatty Liver?
Let's Build a Plan Around Your Body.
Fatty liver is reversible — but what works depends on your specific metabolic profile, not a generic diet plan. In a free 20-minutes consultation with our clinical dietitian, you'll get:
- ✓ A review of your blood reports and current symptoms
- ✓ Clarity on whether your fatty liver has a genetic component
- ✓ A personalised starting point for diet and lifestyle changes
- ✓ Answers to your specific questions — no generic advice
No cost · No commitment · 20 minutes with a clinical dietitian
Related Articles
Share this article
Nupur Sharma
Nupur Sharma is a Sports Nutritionist. She has a scientific approach towards nutrition. She passionately unfolds latent aspects linking nutritional science and sports performance so that athletes and fitness enthusiasts can achieve their highest potential. She holds a Master’s degree in Sports Nutrition and Bachelor’s degree in Food, Nutrition and Dietetics.