Indian Diet Chart for High Cholesterol: Foods to Eat, Avoid & Weekly Meal Plan

Indian Diet Chart for High Cholesterol: Foods to Eat, Avoid & Weekly Meal Plan
⚡ Quick Summary
High Cholesterol: Why Diet Matters More Than You Think
Being from the field of nutrition, I see so many people worried about their blood reports, confused about food, and scared after hearing the words "your cholesterol is high." Many of them feel perfectly fine physically, which makes it even harder to believe that something serious could be going on inside their body.
High cholesterol often doesn't show symptoms early on. No pain, no discomfort, just numbers on a report. And that's exactly why it's dangerous. Over the years, I've seen patients who ignored these numbers thinking "I'll manage it later", only to face serious complications later in life.
Behind the scenes, poor food choices, long sitting hours, stress, lack of sleep, and excess refined carbs slowly start affecting the blood vessels. Over time, cholesterol begins to deposit along the artery walls, narrowing them. Often, the first sign people notice is not a mild warning but something serious like chest discomfort, sudden dizziness, or even fainting due to a cardiac event.
The good news is that dietary changes can significantly improve cholesterol levels, especially when addressed early. And no, you don't need to give up Indian food. In fact, when chosen wisely, Indian meals can be extremely heart-friendly.
This blog will walk you through a practical Indian diet chart for high cholesterol, foods to eat and avoid, blood test markers to monitor, and lifestyle tips that actually work.
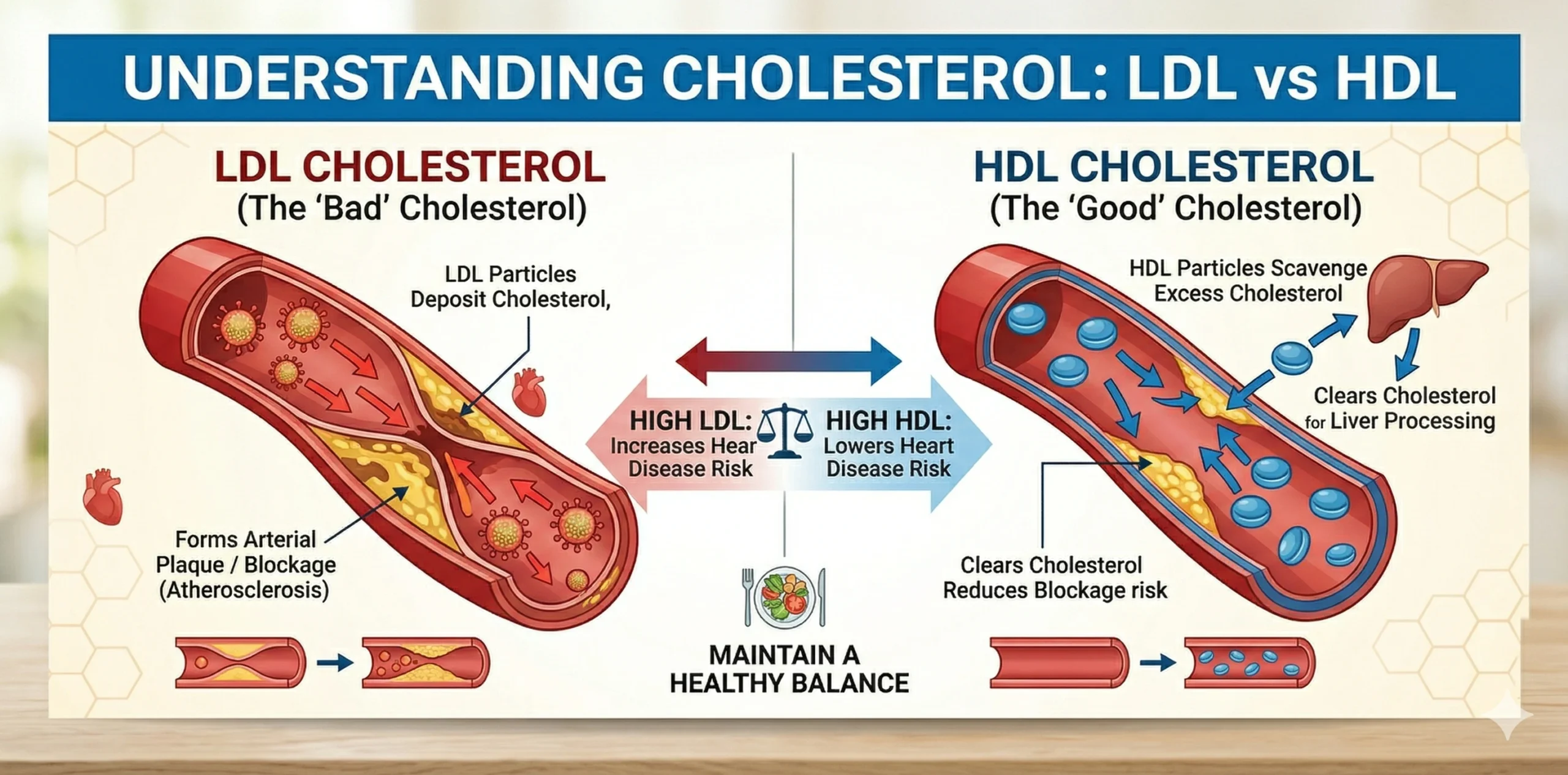
LDL vs HDL — understanding the difference is the first step to managing cholesterol
Understanding Cholesterol: LDL vs HDL Explained
Cholesterol itself is not the villain. It is a fat-like substance that cannot travel freely in the blood, so it needs carriers called lipoproteins. You can think of these lipoproteins as vehicles that transport fat and cholesterol through the bloodstream.
LDL (Low-Density Lipoprotein) — "Bad Cholesterol"
LDL carries cholesterol from the liver to different parts of the body. When present in excess, LDL tends to deposit cholesterol along the artery walls, leading to plaque formation, narrowing of blood vessels, and increased risk of heart disease. This is why LDL is commonly referred to as bad cholesterol.
HDL (High-Density Lipoprotein) — "Good Cholesterol"
HDL works in the opposite direction. It collects excess cholesterol from the arteries and tissues and transports it back to the liver, where it can be broken down and eliminated. This protective role earns HDL the name good cholesterol.
A heart-healthy diet and lifestyle aim to reduce excess LDL and triglycerides while supporting healthy HDL levels, ensuring smoother fat metabolism and better cardiovascular health.
What Does a Healthy Lipid Profile Look Like?
Don't just look at total cholesterol. Your LDL:HDL ratio is a much better indicator of heart disease risk. Ask your doctor to explain this ratio at your next checkup.
| Marker | Ideal Level | Borderline | High Risk |
|---|---|---|---|
| Total Cholesterol | Below 200 mg/dL | 200–239 mg/dL | Above 240 mg/dL |
| LDL (Bad) | Below 100 mg/dL | 130–159 mg/dL | Above 160 mg/dL |
| HDL (Men) | Above 40 mg/dL | 35–40 mg/dL | Below 35 mg/dL |
| HDL (Women) | Above 50 mg/dL | 40–50 mg/dL | Below 40 mg/dL |
| Triglycerides | Below 150 mg/dL | 150–199 mg/dL | Above 200 mg/dL |
| LDL:HDL Ratio | Below 3.5 | 3.5–5.0 | Above 5.0 |
Blood Tests to Check When Cholesterol is High
When cholesterol levels come high, it is important to review the complete lipid profile, not just total cholesterol.
- Total Cholesterol: Desirable level is below 200 mg/dL. This gives an overall picture but should not be interpreted alone.
- LDL Cholesterol (Bad Cholesterol): Ideally below 100 mg/dL. High LDL increases plaque formation in arteries and raises heart disease risk.
- HDL Cholesterol (Good Cholesterol): Protective cholesterol that helps clear excess fat from blood vessels. Ideal levels: above 40 mg/dL in men and 50 mg/dL in women.
- Triglycerides: Normal levels are below 150 mg/dL. Elevated values are commonly linked to excess sugar intake, fatty liver, and sedentary lifestyle.
Want to understand your full metabolic picture? Cholesterol is just one piece. Read our complete guide on which blood tests reveal hidden metabolic issues before symptoms appear.
11 Blood Tests That Reveal Your Metabolic Health →
These 10 Indian foods are clinically proven to reduce LDL and improve your lipid profile
Top 10 Indian Foods That Lower Cholesterol Naturally
These foods are clinically proven to reduce LDL, raise HDL, or lower triglycerides — and all are readily available in Indian kitchens:
Oats (Jaee)
Why: Contains beta-glucan, a soluble fibre that binds to cholesterol in the gut and prevents absorption. Studies show 3g/day of beta-glucan can reduce LDL by 5–10%.
How to eat: Oats upma, oats porridge, oats dosa.
Best for blood sugar & LDLMethi (Fenugreek Seeds)
Why: Galactomannan fibre slows cholesterol absorption; saponins reduce cholesterol synthesis in the liver.
How to eat: Soak 1 tsp overnight, drink water on empty stomach. Add to dal, sabzi, paratha dough.
Best for PCOS & cholesterolFlaxseeds (Alsi)
Why: Rich in omega-3 fatty acids and lignans that lower LDL and reduce inflammation.
How to eat: 1 tbsp ground flaxseeds in dal, roti dough, or buttermilk daily. Always grind before eating — whole seeds pass through undigested.
Best for LDL & inflammationWalnuts (Akhrot)
Why: Highest omega-3 content among all nuts. Reduces LDL and improves artery flexibility.
How to eat: 5–7 walnuts daily as a snack. Avoid salted or roasted.
Best morning snackRajma (Kidney Beans)
Why: High in soluble fibre and plant sterols that block cholesterol absorption.
How to eat: Rajma curry 2–3 times per week. Avoid adding excess ghee or cream.
Best for fibre intakeAmla (Indian Gooseberry)
Why: Rich in Vitamin C and antioxidants that prevent LDL oxidation. Oxidised LDL is what causes arterial plaque.
How to eat: 1 fresh amla daily, amla juice, or amla powder in warm water each morning.
Best anti-oxidant foodGarlic (Lehsun)
Why: Allicin compound reduces LDL production in the liver and mildly lowers blood pressure.
How to eat: 1–2 raw garlic cloves daily on empty stomach, or add liberally to cooking.
Best for blood pressure tooTofu / Soybean / Soy Milk
Why: Soy protein directly reduces LDL. 25g/day of soy protein can lower LDL by 5–6%.
How to eat: Tofu sabzi, soy milk, soybean curry.
Best plant proteinMustard / Rice Bran Oil
Why: Low in saturated fat, high in MUFA and PUFA. Mustard oil's erucic acid has been shown to improve lipid profiles in Indian populations specifically.
How to use: 3–4 tsp per day for cooking. Rotate between mustard and rice bran oil.
Best cooking oil swapGreen Tea
Why: Catechins reduce LDL and total cholesterol. 2–3 cups/day shows measurable results within 8 weeks.
How to drink: Without milk or sugar. Add a squeeze of lemon for better absorption.
Best daily habit7-Day Indian Diet Chart for High Cholesterol
This meal plan keeps total fat under 30% of calories, saturated fat under 7%, and includes at least 25–30g of fibre daily — the two most important dietary targets for cholesterol management.
Health Risks and Complications of High Cholesterol
High cholesterol is not just a "numbers problem" on a lab report. If left unmanaged, it can lead to serious health complications.
1. Heart Attack (Myocardial Infarction)
Excess LDL cholesterol forms plaque inside arteries. When these plaques rupture, they can block blood flow to the heart, leading to a sudden heart attack. This is why we often hear about people collapsing or fainting suddenly without prior warning.
2. Stroke
Blocked or narrowed arteries supplying blood to the brain can result in a stroke, affecting speech, movement, memory, or vision.
3. Atherosclerosis (Hardening of Arteries)
Cholesterol buildup makes arteries stiff and narrow, forcing the heart to work harder. Over time, this increases blood pressure and cardiac strain.
4. Poor Circulation
Reduced blood flow can cause:
- Leg pain while walking
- Cold hands and feet
- Fatigue and breathlessness
5. Metabolic Complications
High cholesterol often travels with:
- Fatty liver
- Insulin resistance
- Type 2 diabetes
- Obesity
These conditions are closely interconnected — together they form what is known as metabolic syndrome. Read our complete guide to understand how these conditions reinforce each other and how to reverse them naturally.
Complete Guide to Metabolic Health: Causes, Symptoms & Reversal →Diet Principles to Reduce High Cholesterol Naturally
Before jumping into a meal plan, it's important to understand a few key principles:
- Increase soluble fibre — binds cholesterol and removes it from the body
- Choose healthy fats instead of saturated and trans fats
- Limit refined sugars and processed foods
- Prefer whole, minimally processed Indian foods
Indian Diet Plan for High Cholesterol
🌅 Early Morning
- Warm water with soaked methi seeds (fenugreek)
- 5–6 soaked almonds or walnuts
🍽 Breakfast
- Vegetable oats upma
- Moong dal chilla with mint chutney
- Ragi idli with sambar (less coconut, more vegetables)
- Namkeen dalia
☀️ Mid-Morning Snack
- One fruit (papaya, orange, apple, berries)
- Coconut water
- Sprouts chaat (steamed, not fried)
- Buttermilk
🌿 Lunch
- 1–2 multigrain rotis OR small portion of brown rice
- One bowl of dal, rajma, chole, or curd
- One vegetable sabzi (preferably steamed or sautéed lightly)
- Raw salad (cucumber, carrot, beetroot)
🫖 Afternoon Snack
- Roasted makhana
- Roasted chana
- Green tea or herbal tea
- Handful of nuts and seeds (flaxseed, sunflower seeds)
🌙 Dinner
- Vegetable dal with one multigrain roti
- Tofu or paneer (low-fat) sabzi with multigrain roti
- Vegetable khichdi with moong dal
- Quinoa vegetable khichdi
Foods to Avoid or Limit in High Cholesterol
To manage cholesterol effectively, reduce or avoid:
- Fried foods and fast foods
- Bakery items (cakes, pastries, cookies)
- Vanaspati, margarine, trans fats
- Red meat and processed meats
- Full-fat dairy (cream, butter, cheese)
- Sugary drinks and desserts
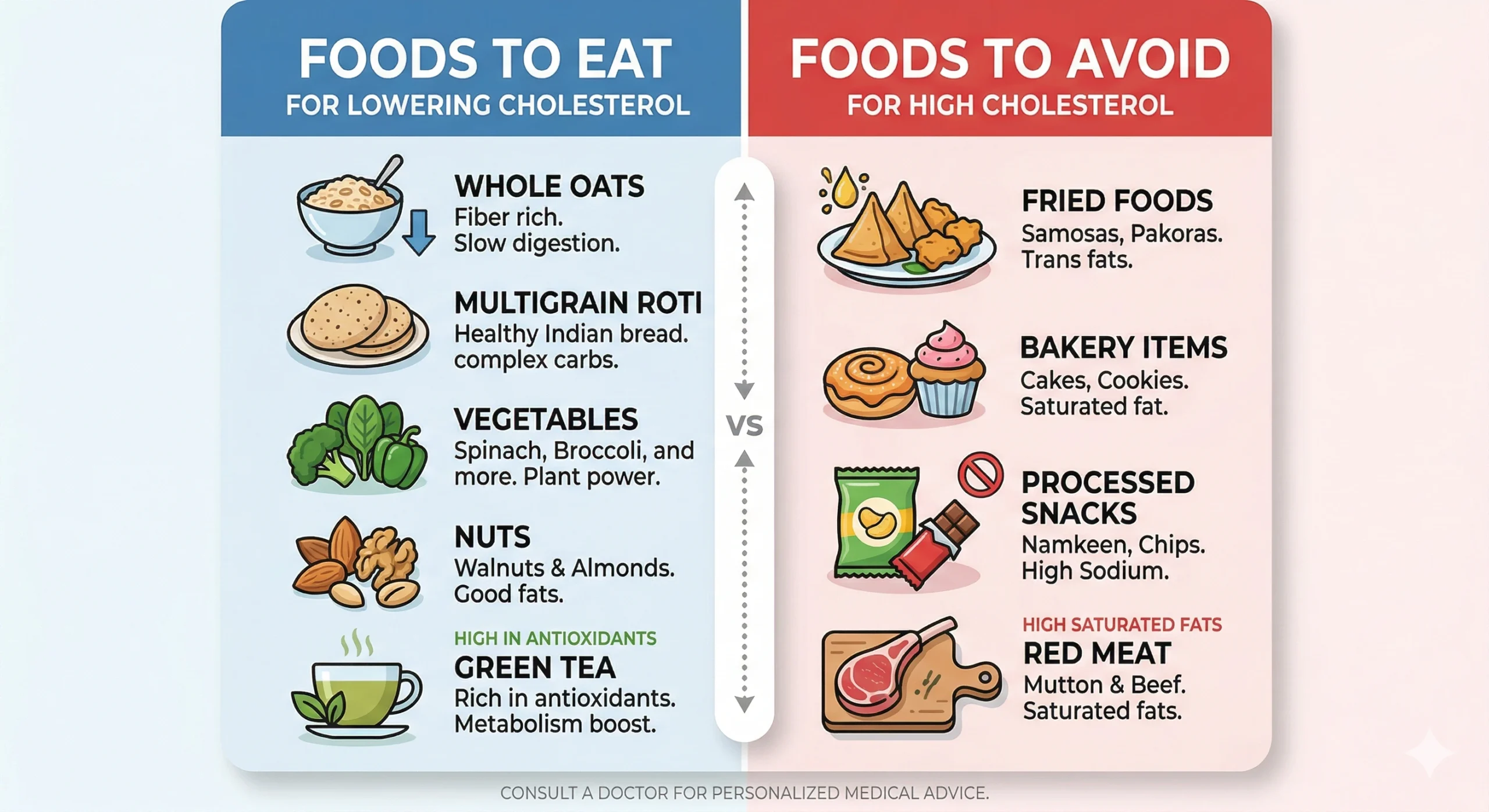
A quick visual guide to foods that help vs harm your cholesterol levels
Foods to Eat vs Avoid: Quick Reference Table
| Category | ✅ Eat Freely | ❌ Avoid / Limit |
|---|---|---|
| Grains | Oats, ragi, bajra, brown rice, multigrain roti | Maida, white bread, biscuits, namkeen, instant noodles |
| Proteins | Dal, rajma, chana, tofu, low-fat curd, egg whites, soy | Red meat, sausages, full-fat paneer, fried eggs, cream |
| Fats & Oils | Mustard oil, rice bran oil, olive oil, flaxseeds, walnuts, almonds | Vanaspati, dalda, butter, excess coconut oil, ghee (limit to 1 tsp/day) |
| Vegetables | All vegetables, especially leafy greens, broccoli, garlic, onion | Avoid deep-frying any vegetables |
| Fruits | Apple, papaya, orange, berries, guava, amla, pear | Mango & chikoo (limit), banana (limit), packaged fruit juices |
| Dairy | Low-fat curd, skimmed milk, buttermilk, limited paneer | Full-fat milk, cream, cheese, ice cream, khoya |
| Beverages | Green tea, herbal tea, coconut water, buttermilk, plain water | Sugary drinks, packaged juices, alcohol, excess full-fat milk chai |
Is Your Cholesterol Linked to Your Genes?
Some people follow a perfect diet and still struggle with high cholesterol. In many cases, the answer lies in your DNA. Find out your metabolic type in 3 minutes.
Take the Free Metabolic Quiz →No signup required · 3-minute quiz · Instant results
Lifestyle Changes to Lower Cholesterol Levels
Diet alone cannot do all the work when it comes to managing high cholesterol. It must be supported by consistent lifestyle habits. Regular physical activity, especially cardio-based exercises such as brisk walking, cycling, swimming, jogging, or dancing, plays a crucial role in cholesterol management. Cardio exercises help the body burn excess circulating fats, lower LDL and triglyceride levels, and improve HDL (good cholesterol) by enhancing fat metabolism and improving blood circulation. Aim for at least 30–45 minutes of moderate-intensity activity on most days of the week.
Equally important is adequate sleep. Getting 7–8 hours of quality sleep each night helps regulate hormones involved in fat metabolism and prevents insulin resistance, both of which influence cholesterol levels. Chronic sleep deprivation can raise LDL and triglycerides over time.
Stress management is another often-overlooked factor. Persistent stress increases cortisol levels, which can negatively affect lipid profiles. Practices such as yoga, meditation, deep breathing, or mindful movement help calm the nervous system and support heart health. See how high cortisol slows your metabolism →
Lastly, lifestyle risks such as smoking and excessive alcohol intake should be avoided. Smoking lowers HDL and damages blood vessels, while excess alcohol can raise triglycerides and contribute to fatty liver, further worsening cholesterol levels.
How Long Does It Take to Lower Cholesterol with Diet?
Most people want to know: "How quickly will I see results?" Here is a realistic timeline based on clinical observations:
1–2
Digestive improvements begin
Less bloating, better gut health, improved energy levels. No visible change in cholesterol numbers yet — this is normal.
3–4
Triglycerides start dropping
Especially if cutting sugar. Some improvement in blood sugar levels. First measurable LDL reduction possible if changes are consistent.
6–8
10–20% LDL reduction
Most people see meaningful improvement. HDL may start rising slightly with regular exercise. Total cholesterol typically drops 15–30 mg/dL.
3–6
Full dietary benefit visible
Those with mild-moderate elevation often reach target ranges. Those with genetic or severe cholesterol may need additional medical support.
Can Genetics Cause High Cholesterol?
In some individuals, high cholesterol may be influenced by genetic factors. Certain genes affect how the body produces, transports, and clears cholesterol, which can lead to persistently high levels despite lifestyle efforts.
If cholesterol levels remain elevated or there is a strong family history of heart disease, a DNA-based genetic test can help identify inherited risk factors. This provides deeper insight into how the body responds to fats and allows for more personalised nutrition and lifestyle planning.
For those seeking more clarity, you can book a consultation with us to know more.
Is your body ageing faster than your real age? High cholesterol, insulin resistance, and poor metabolic health can accelerate biological ageing. Learn how nutrition and lifestyle impact your metabolic age.
Metabolic Age vs Real Age: What Yours Says About Your Health →Frequently Asked Questions
High cholesterol usually does not show obvious symptoms. Many people feel perfectly healthy even with elevated levels. That's why regular blood tests — at least once a year — are essential for early detection.
Not always. While poor dietary habits, sedentary lifestyle, and stress play a major role, genetics can also influence cholesterol levels. Some individuals may have inherited risk factors that require more personalized interventions.
For heart health, choose oils that are low in saturated fats and rich in healthy fats. Good options include mustard oil, rice bran oil, soybean oil, and olive oil. Limit ghee, butter, and vanaspati. Use minimal oil during cooking and prefer methods like steaming, grilling, or sautéing over deep-frying.
For adults, a lipid profile test once a year is usually sufficient. If there is a family history of heart disease or other risk factors, testing every 6 months may be advisable. If you have already been diagnosed with high cholesterol, it is recommended to check your levels every 3–4 months to monitor progress and make timely adjustments to your diet and lifestyle.
Yes, cholesterol levels — especially LDL (bad cholesterol) — can be significantly reduced through diet and lifestyle changes in many people. A diet rich in whole grains, fruits, vegetables, legumes, nuts, seeds, and healthy fats helps lower LDL cholesterol while supporting heart health.
In an Indian context, replacing refined carbs, fried foods, excess ghee/butter, and sugary items with fiber-rich foods like oats, millets, dal, vegetables, fruits, and fermented foods (curd) can lead to noticeable improvements within a few weeks.
The time required varies from person to person, but many people start seeing improvements within 4 to 8 weeks of making consistent dietary and lifestyle changes. Adopting a heart-healthy diet, increasing physical activity, improving sleep, and managing stress can gradually lower LDL and improve overall lipid profiles.
For individuals with mild to moderately high cholesterol, meaningful reductions can be seen within a few months. However, people with very high cholesterol, genetic conditions, diabetes, or existing heart disease may require a longer duration and sometimes medical treatment in addition to diet. Regular blood tests every 8–12 weeks help track progress.
Ghee in small amounts (1 tsp/day) is not harmful and may even support digestion. The problem arises when ghee is used in large quantities — 2–3 tbsp/meal, which is common in many Indian households. At high quantities, ghee raises LDL due to its saturated fat content. Replace excess ghee with mustard oil or rice bran oil for everyday cooking, and use ghee only as a finishing flavour.
Yes, but choose wisely. White rice in large portions raises blood sugar quickly, which indirectly elevates triglycerides. Switch to brown rice or millets (bajra, jowar, ragi) for most meals. If you prefer white rice, reduce the portion to 1 small katori per meal and pair it with plenty of dal, vegetables, and curd to slow glucose absorption.
Fresh coconut in small amounts is fine. Coconut oil, however, is high in saturated fat and can raise LDL with regular use. Use it sparingly for tadka or flavouring — not as your primary cooking oil. Coconut water is perfectly safe and actually supports hydration and heart health.
Yes. Yoga reduces cortisol (stress hormone) which directly influences cholesterol levels. Studies show that regular yoga practice — especially Surya Namaskar, Pranayama, and Shavasana — can reduce total cholesterol and LDL by 5–10% over 3–6 months. Combine yoga with brisk walking for the best results.
Top 3 Indian breakfasts for cholesterol management:
- Vegetable oats upma — high beta-glucan fibre
- Moong dal chilla — high plant protein, low fat
- Ragi idli with sambar — high fibre, fermented, cholesterol-friendly
Avoid: puri, paratha with butter, white bread toast with jam, and packaged cereals with added sugar.
Related Articles
Share this article
Nupur Sharma
Nupur Sharma is a Sports Nutritionist. She has a scientific approach towards nutrition. She passionately unfolds latent aspects linking nutritional science and sports performance so that athletes and fitness enthusiasts can achieve their highest potential. She holds a Master’s degree in Sports Nutrition and Bachelor’s degree in Food, Nutrition and Dietetics.