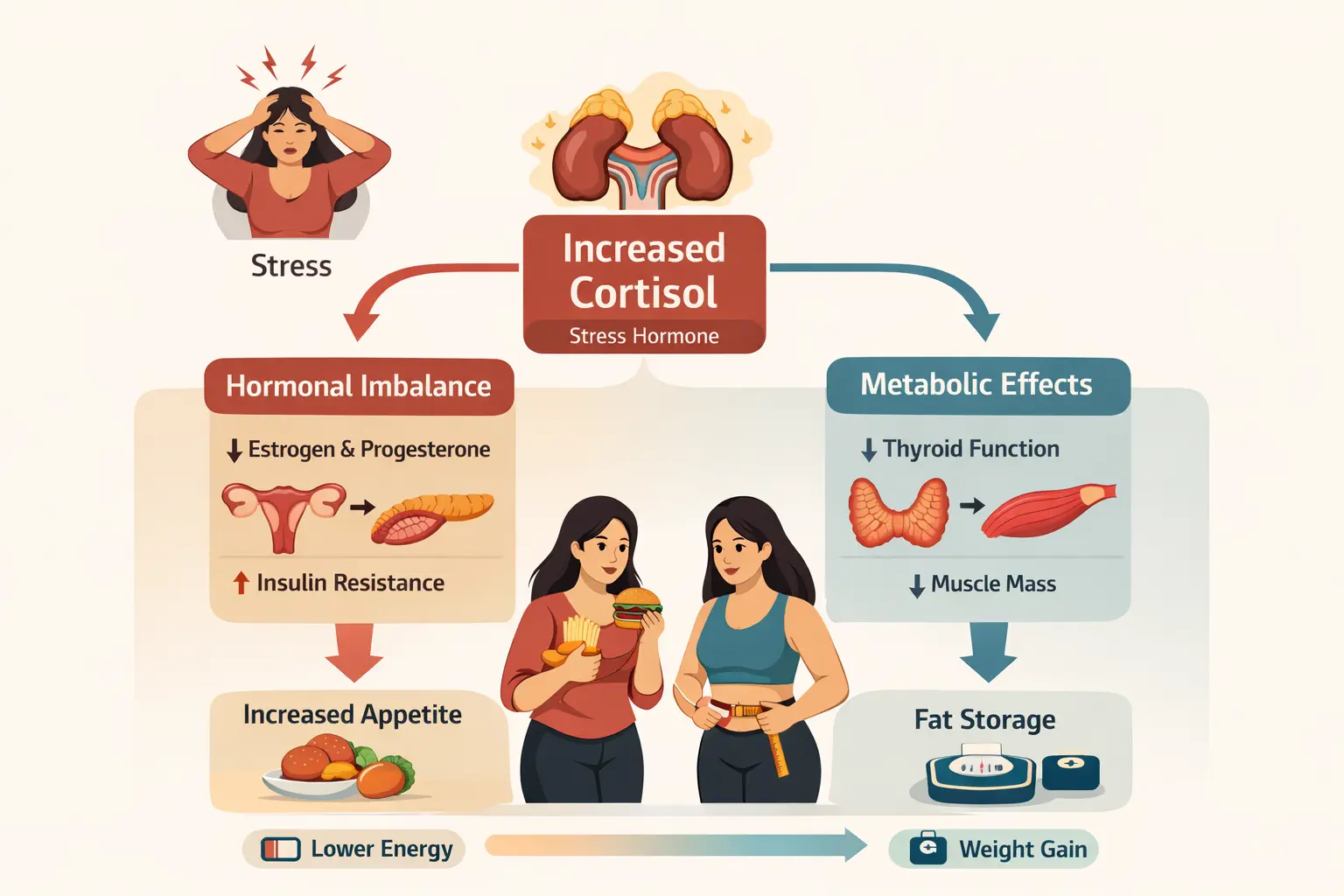
How Misleading Lab Results Can Affect Your Diabetes Diagnosis
High HbA1c levels may not always indicate diabetes, as they can be influenced by factors like vitamin B12 deficiency. Understanding the underlying causes is crucial for accurate diagnosis and effective treatment.
How Are Numbers Used to Diagnose Diabetes?
In the world of modern medicine, numbers are treated as absolute truth. A blood report arrives. A few values are highlighted in red. A diagnosis is formed. A treatment plan begins. This process is so standardized that most patients rarely question it. In fact, many healthcare systems are built on the assumption that laboratory numbers reflect reality with near-perfect accuracy.
If your HbA1c is high, the conclusion seems obvious: your blood sugar has been high, and you are on the path toward diabetes. But what if the numbers are technically correct… and the diagnosis is fundamentally wrong?
What if the marker being used to diagnose diabetes is elevated not because of high blood sugar, but because of something entirely different happening inside the body?
What if the number is high not because sugar is elevated, but because your body's renewal system has slowed down?
This is not a theoretical discussion. This is a real and increasingly common scenario. It is the story of a High Impact Problem that remained undetected, leading to a treatment plan that appeared logical on paper but actually made the patient feel worse. This is the story of the diabetes misdirection.
What Does a Textbook "Diabetic" Presentation Look Like?
Modern medicine relies heavily on biomarkers. These markers are measurable indicators of health or disease. They allow doctors to make decisions quickly and efficiently.
One of the most widely used markers for diagnosing diabetes is HbA1c. HbA1c represents the amount of sugar attached to haemoglobin in red blood cells. Since red blood cells live for several months, HbA1c gives an estimate of average blood sugar levels over time.
Because of this, HbA1c has become one of the most trusted indicators in metabolic medicine.
But there is an important truth that often goes unnoticed. HbA1c does not measure blood sugar directly. It measures the sugar coating on red blood cells. And that distinction can change everything.
The patient arrived with a set of symptoms that many doctors encounter every single day. The complaints were common, almost routine. But together, they formed a pattern that seemed unmistakable. The patient reported:
- Persistent fatigue that did not improve with rest
- Brain fog and difficulty concentrating
- Unexplained weight gain
- Intense cravings for sugary foods
- Elevated HbA1c levels
- High triglycerides
On paper, this looked like a classic case of insulin resistance. The symptoms aligned with the lab markers. The lab markers aligned with standard diagnostic criteria. Everything pointed in one direction:
High HbA1c → High blood sugar → Insulin resistance → Pre-diabetes or diabetes.
To confirm the diagnosis, the patient underwent additional tests — a glucose overload test, which surprisingly came back normal, and an insulin resistance test, which was only slightly elevated. Despite these mixed results, the presence of high HbA1c and triglycerides was enough to keep the diagnosis on the metabolic track. So the patient was placed on a Standard Care Path.
What Is the Standard Care Path for Diabetes Management?
The treatment plan followed established clinical guidelines. It was safe, conventional, and widely accepted. The patient was advised to:
- Follow a low-carbohydrate, low-fat diet
- Begin a routine of brisk daily walking
- Start medications to control cholesterol
- Take medications to regulate blood sugar
The expected outcome was straightforward: HbA1c levels would drop, body weight would decrease, energy levels would improve, and overall metabolic health would get better. From a clinical standpoint, nothing about this approach was unusual. Everything seemed correct — until the follow-up results arrived.
What Happens When Following Diabetes Treatment Makes You Worse?
After following the advice diligently, the patient returned for a follow-up. The results were confusing. Some markers had improved — average blood glucose levels had decreased and cholesterol levels were better. But two major problems appeared:
- HbA1c had increased instead of decreasing
- Fatigue had worsened significantly
This created a paradox. The patient was doing everything right. The numbers should have improved across the board. Yet the HbA1c moved in the wrong direction, and the patient felt worse than before. In many conventional settings, this situation leads to one response: increase medication doses, restrict carbohydrates further, and add additional glucose-lowering interventions. But this is where the concept of the High Impact Problem becomes essential.
The Danger of Treating a "Snapshot"
Most diagnostic systems rely on what can be called a snapshot approach. A blood test captures a moment in time. The values are compared to a reference range. If a number is high, the system assumes the associated disease must be present.
But the human body is not a snapshot. It is a dynamic system. Numbers are outcomes of processes. They are not the processes themselves. When a number is abnormal, it is the result of something happening beneath the surface. If you treat the number without understanding the process behind it, you may end up treating the wrong problem entirely. That is exactly what happened in this case. The focus was entirely on lowering glucose — but the body was signalling a deeper dysfunction that had nothing to do with sugar.
What Is the High Impact Problem Related to B12 Deficiency?
The turning point came when the patient underwent a more comprehensive evaluation at Unlock.fit. Instead of relying solely on standard lab markers, the analysis included functional blood test interpretation and DNA-based metabolic analysis.
This deeper investigation revealed something unexpected. The primary issue was not sugar. It was functional anaemia caused by a significant vitamin B12 deficiency and poor metabolism of iron and B12. This discovery completely changed the interpretation of the patient's lab results.
How Can a B12 Deficiency Mislead a Diabetes Diagnosis?
HbA1c measures the amount of sugar attached to haemoglobin inside red blood cells over time. This means the test depends on two major factors: the level of sugar in the blood, and the lifespan of the red blood cells. Most people only consider the first factor. But the second one is equally important.
Delayed Renewal: Vitamin B12 is essential for the production of red blood cells in the bone marrow. Without adequate B12, red blood cell production slows down and the body cannot replace old cells efficiently.
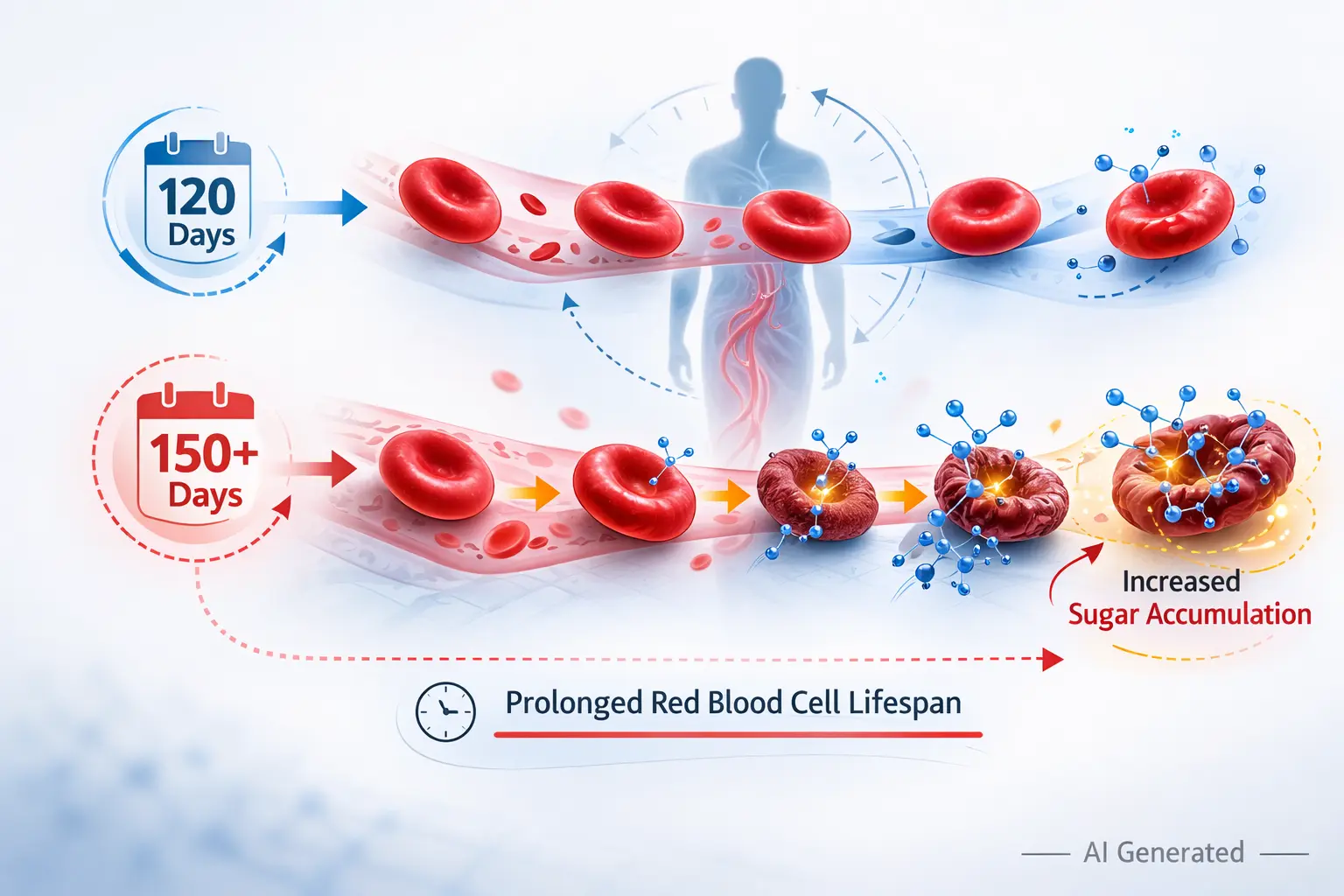
Extended Lifespan of Old Cells: In a healthy individual, a red blood cell lives for about 120 days. But in a person with B12 deficiency, older cells remain in circulation longer. In this patient, red blood cells were staying in the system for more than 150 days.
The Glycation Trap: HbA1c measures how much sugar has attached to red blood cells over their lifetime. The longer a cell lives, the more sugar it accumulates. So even if blood sugar levels are normal, older cells will show more glycation and HbA1c will appear higher. The number is technically correct — but the interpretation is wrong.
The Mitochondrial Collapse: Vitamin B12 plays a crucial role in energy production, fat metabolism, nervous system health, and mitochondrial function. When B12 is low, cells cannot efficiently convert fat into energy, mitochondrial efficiency drops, and the nervous system becomes stressed. This explains why the patient felt more exhausted even while eating a healthier diet. The problem was not the fuel — it was the engine.
How Do Standard Care and Root Cause Approaches Differ?
| Category | Standard Care Path | Root Cause Path |
|---|---|---|
| Core Question | What is the abnormal marker? | What system is actually malfunctioning? |
| Primary Focus | Reduce elevated HbA1c numbers | Identify and fix the underlying cause |
| Interventions Used | Diet changes, medications, exercise | B12 supplementation, correcting deficiency |
| Treats Root Cause | No | Yes |
| B12 Deficiency | Remained untreated | Identified and corrected |
| Red Blood Cell Turnover | Remained abnormal | Normalized after B12 correction |
| HbA1c Outcome | Potentially improved artificially | Normalized naturally |
| Fatigue | Worsened over time | Energy levels improved |
| Nervous System Stress | Continued unaddressed | Resolved with B12 correction |
| Mitochondrial Function | Not addressed | Improved with B12 correction |
| Glucose Management | Artificially suppressed | No suppression needed — body self-corrected |
| Long-Term Outcome | Deeper problem remains | Underlying issue fully resolved |
Why This Matters More Than You Think
This scenario is not rare. Many people today are labelled prediabetic or diabetic, follow strict diets, take medications, yet continue to feel tired, foggy, and unwell. In some of these cases, the issue is not sugar at all. It may be nutrient deficiencies, hormonal imbalances, mitochondrial dysfunction, or genetic metabolic variations. But these causes remain hidden if the system only looks at surface-level numbers. These misinterpretations are often connected to the 6 core factors that drive women's metabolic and hormonal health.
What Is The Solution? The Triangulation Approach
To avoid diagnostic misdirection, health must be viewed from multiple angles. At Unlock.fit, this approach is called triangulation. It involves three levels of understanding.
- Level 1 — Symptoms (The Surface): Fatigue, cravings, weight gain, brain fog. These are signals that something is wrong, but symptoms alone cannot reveal the cause.
- Level 2 — Blood Reports (The Snapshot): HbA1c, triglycerides, vitamin levels, iron markers. These numbers must be interpreted in context — they are snapshots, not full stories.
- Level 3 — Genetic Blueprint (The Context): Your DNA determines how you absorb nutrients, metabolize vitamins, and handle fats and sugars. Two people can have identical lab reports but completely different root causes.
| Level | Diagnostic Layer | Type | Key Markers / Indicators | What It Reveals | Limitation |
|---|---|---|---|---|---|
| Level 1 | Symptoms | Surface Signals | Fatigue, Cravings, Weight Gain, Brain Fog | Signals that something is wrong | Cannot reveal the root cause on its own |
| Level 2 | Blood Reports | Measurable Snapshot | HbA1c, Triglycerides, Vitamin Levels, Iron Markers | Quantifiable data on body markers | Numbers must be interpreted in context — not the full story |
| Level 3 | Genetic Blueprint | Root Context | Nutrient absorption, Vitamin metabolism, Mitochondrial function, Fat & sugar processing | Why two people with identical labs can have different root causes | Requires integration with symptoms and blood data for full picture |
What Is the Bigger Lesson About Diabetes Diagnosis?
This case reveals a powerful truth: not every high HbA1c is diabetes. Not every metabolic symptom is caused by sugar. And not every lab result tells the full story. Sometimes the body is not suffering from excess — it is suffering from deficiency. And when the system treats a deficiency as if it were an excess, the results can be confusing, frustrating, and even harmful.
True health is not about guessing from vague signals. It is about understanding the unique biology of each individual. When we combine symptoms, functional blood data, and genetic insights, we stop treating numbers — and start treating the system itself. That is the difference between managing disease and restoring health.
Frequently Asked Questions
Final Takeaway
If stress, sleep, or metabolic concerns feel persistent, a personalised approach can help. A free consultation with Unlock.fit can help you understand how your hormones, nutrition, and lifestyle interact — including insights from DNA and blood markers — to support long-term metabolic health. To understand the full picture, explore the core factors that shape women's health and how they connect to conditions like insulin resistance.
Book Your Free Consultation
Share this article
Tavleen
Meet Tavleen, a "human coder" driven by an insatiable passion for genetics that's anything but ordinary. She believes that real change starts at the roots of who we are, and that's precisely why she delved headfirst into the intricate world of Nutrigenomics during her pursuit of a master's degree. But Tavleen's journey doesn't stop there – she's a biohacker extraordinaire, dedicated to unraveling the secrets of how the food we consume can spark astonishing transformations within the tiniest corners of our bodies. Get ready to embark on a captivating exploration of the intersection between genetics, nutrition, and the endless possibilities it holds. Tavleen's unique perspective promises to shed light on the awe-inspiring world of personalised health, and you won't want to miss a single word of her exciting discoveries.