The Complete Guide to Metabolic Health: Causes, Symptoms and How to Reverse It Naturally
The Complete Guide to Metabolic Health: Causes, Symptoms and How to Reverse It Naturally
⚡ Quick Answer
Metabolic health refers to how well your body manages energy, blood sugar, fat metabolism, and hormonal balance. Poor metabolic health develops gradually through insulin resistance, chronic inflammation, nutrient deficiencies, and lifestyle factors. The good news: metabolic dysfunction can be reversed naturally through the 6 pillars of metabolic health restoration - blood sugar management, visceral fat reduction, gut health support, sleep optimization, lipid management, and addressing nutrient deficiencies with genetic insights.
Have you ever wondered why some people feel energetic, maintain stable weight, and rarely struggle with blood sugar issues, while others experience constant fatigue, weight gain, or metabolic disorders despite similar lifestyles? The answer often lies in metabolic health, a critical yet frequently overlooked aspect of overall well-being.
Metabolic health refers to how efficiently your body processes and uses energy from the food you eat. It involves several interconnected systems that regulate blood sugar levels, convert nutrients into usable energy, burn stored fat, and maintain hormonal balance. When these systems function optimally, the body is able to maintain steady energy levels, balanced glucose levels, and healthy fat metabolism.
However, when metabolic health begins to decline, the body's ability to manage energy becomes impaired. This can lead to issues such as insulin resistance, abnormal fat storage, and hormonal disruptions. Over time, poor metabolic health becomes the underlying driver of many chronic conditions, including type 2 diabetes, fatty liver disease, hormonal imbalances, and persistent fatigue. Because these changes often develop gradually and silently, understanding metabolic health is one of the most important steps toward preventing long-term disease and maintaining overall vitality.
The Complete Guide to Metabolic Health
Metabolic health is the foundation of long-term health and disease prevention, yet it is often overlooked until a medical diagnosis forces attention to it. Many of the most common chronic conditions today, such as diabetes, fatty liver disease, heart disease, and hormonal disorders, they do not appear suddenly. They develop gradually as a result of underlying metabolic dysfunction that can progress silently for years.
The challenge is that most people wait until symptoms appear or a lab report shows abnormal results before they begin to address their health. By that time, metabolic imbalances like insulin resistance, chronic inflammation, and lipid abnormalities may have already been developing for a long period. Understanding metabolic health early allows individuals to recognize warning signs, identify risk factors, and take preventive action before serious disease develops.
What Is Metabolic Health?
Metabolic health refers to how well the body regulates and maintains key biochemical processes involved in energy balance, fat metabolism, blood sugar control, and cardiovascular function. Clinically, metabolic health is commonly assessed using five key markers: fasting blood glucose, triglycerides, high-density lipoprotein (HDL) cholesterol, blood pressure, and waist circumference. When all five of these markers fall within healthy ranges, the body is considered metabolically healthy because it indicates efficient insulin function, balanced lipid metabolism, and minimal systemic inflammation. However, if even a few of these markers are abnormal such as elevated triglycerides, increased abdominal fat, or high fasting glucose, the body begins to show signs of metabolic dysfunction, which significantly raises the risk of chronic diseases such as type 2 diabetes, cardiovascular disease, and fatty liver disease.
Importantly, metabolic health is not determined by just one marker or by body weight alone. All five parameters must be within healthy ranges simultaneously to indicate true metabolic balance. For example, a person may have normal blood sugar but elevated triglycerides and central obesity, which still signals underlying metabolic risk. This cluster of abnormalities is often referred to as metabolic syndrome, a condition that substantially increases the likelihood of developing diabetes and cardiovascular disease.
In the Indian context, the burden of poor metabolic health is particularly concerning. Studies show that metabolic syndrome affects roughly 30% of adults in India, with higher prevalence in urban populations due to sedentary lifestyles, processed food consumption, and increased stress. Even more alarming, national data suggest that over 70% of Indian adults may be metabolically unhealthy, including many individuals who appear lean but have hidden metabolic abnormalities such as insulin resistance or abnormal lipid levels. This phenomenon, often described as the "thin-outside-fat-inside" metabolic phenotype, highlights why routine metabolic screening and lifestyle interventions are essential for early prevention.
To understand the full picture, explore the core factors that shape women's health and why women's health needs a different approach when it comes to metabolism and hormones.
What Causes Metabolic Dysfunction?
Metabolic dysfunction usually doesn't appear overnight, it develops slowly as multiple factors begin to disrupt the body's ability to manage energy efficiently. At the center of this process is insulin resistance, one of the most common root drivers of metabolic imbalance. Insulin is the hormone responsible for helping glucose move from the bloodstream into cells where it can be used for energy. When cells become less responsive to insulin, the body has to produce more of it to keep blood sugar stable. Over time, this can lead to chronically elevated blood sugar, increased fat storage, especially around the abdomen and a higher risk of conditions such as prediabetes and type 2 diabetes.
Another major contributor is chronic low-grade inflammation and oxidative stress. Unlike acute inflammation, which is part of the body's natural healing response, chronic inflammation quietly damages cells and tissues over time. This persistent inflammatory state interferes with insulin signaling, disrupts lipid metabolism, and accelerates cellular aging. Diets high in refined carbohydrates, ultra-processed foods, and unhealthy fats, combined with high stress levels, can further fuel this inflammatory environment.
Nutrient deficiencies are also an often-overlooked factor in metabolic health. Essential nutrients such as vitamin B12, iron, vitamin D, and omega-3 fatty acids play critical roles in energy production, mitochondrial function, hormone regulation, and inflammation control. When these nutrients are insufficient which is surprisingly common due to modern diets, gut health issues, or absorption problems the body's metabolic pathways cannot function optimally.
Lifestyle habits also have a profound impact. Poor sleep quality and chronic sleep deprivation can disrupt hormones that regulate appetite, insulin sensitivity, and stress responses. At the same time, a sedentary lifestyle reduces muscle activity, which is one of the body's most important systems for using glucose efficiently. When muscles are underused, the body becomes less effective at clearing glucose from the bloodstream, further contributing to insulin resistance.
Finally, genetic predisposition plays a role in why metabolic dysfunction affects individuals differently. Two people may follow very similar diets and lifestyles, yet one may develop metabolic issues while the other does not. This is because certain genetic variations influence how the body processes carbohydrates, metabolizes fats, regulates inflammation, and absorbs nutrients. Understanding these genetic tendencies can provide valuable insight into why certain metabolic patterns develop and how they can be addressed more effectively through personalized nutrition and lifestyle strategies.
Signs and Symptoms of Poor Metabolic Health
Poor metabolic health often doesn't appear overnight; it usually shows up through subtle signals that many people overlook or normalize.

| Sign of Poor Metabolic Health | Explanation |
|---|---|
| Persistent fatigue or brain fog | Feeling tired even after a full night's sleep or struggling to maintain focus throughout the day. |
| Unexplained weight gain (especially abdominal) | Weight gain around the abdominal area often linked to insulin resistance and hormonal imbalances rather than simply excess calorie intake. |
| Frequent sugar cravings and energy crashes after meals | Feeling energized immediately after eating but quickly experiencing fatigue, irritability, or hunger again within a short period, indicating unstable blood sugar levels and poor metabolic regulation. |
| Abnormal blood test markers | Routine blood tests may reveal high triglycerides, elevated HbA1c, or abnormal cholesterol levels even before clear symptoms develop. |
| Hormonal imbalances | Conditions such as PCOS, thyroid irregularities, and mood fluctuations are often closely connected to underlying metabolic disturbances. |
| Early metabolic dysfunction signals | These symptoms often appear years before more serious metabolic conditions develop, making early recognition important. |
These symptoms are often connected to hormonal imbalance and high cortisol levels that affect metabolism.
How Metabolic Health Is Diagnosed
Diagnosing metabolic health isn't based on just one number or a single test. Instead, it involves looking at a group of blood markers that together give a clearer picture of how your metabolism is functioning. Some of the most tracked markers include fasting blood glucose, HbA1c, triglycerides, HDL cholesterol, fasting insulin, and inflammatory markers like hs-CRP. These tests help identify whether your body is managing blood sugar efficiently, how your lipid metabolism is functioning, and whether there is underlying inflammation contributing to metabolic stress.
Many people assume that HbA1c alone is enough to assess metabolic health, but that's not always the case. HbA1c reflects your average blood sugar levels over the past three months, but it doesn't always capture early metabolic dysfunction. Someone can have a normal HbA1c while still experiencing insulin resistance, high triglycerides, or significant blood sugar fluctuations throughout the day. This is why looking at a broader set of metabolic markers provides a completer and more accurate picture.
Another important aspect is how these blood markers are interpreted. Standard medical ranges are designed primarily to diagnose disease, not to detect early metabolic risk. Functional or preventive interpretations often use tighter optimal ranges to identify imbalances much earlier, before they progress into full-blown metabolic disorders. This approach allows for earlier lifestyle interventions and more personalized health strategies.
In recent years, DNA testing has also become a valuable tool in understanding metabolic risk. Genetic insights can reveal how your body processes carbohydrates, fats, and nutrients, as well as how you respond to inflammation, stress, and exercise. While genes do not determine your destiny, they can provide useful guidance in tailoring nutrition, lifestyle, and preventive strategies to support better metabolic health.
The 6 Pillars of Metabolic Health Restoration
Improving metabolic health is not about following a single diet or relying on one lifestyle change. Instead, it requires addressing multiple interconnected systems in the body. Think of metabolic health as a structure supported by several pillars, when one pillar weakens, the entire system becomes unstable. Restoring metabolic balance involves strengthening these key areas so that blood sugar regulation, fat metabolism, hormonal function, and energy production can work together efficiently.
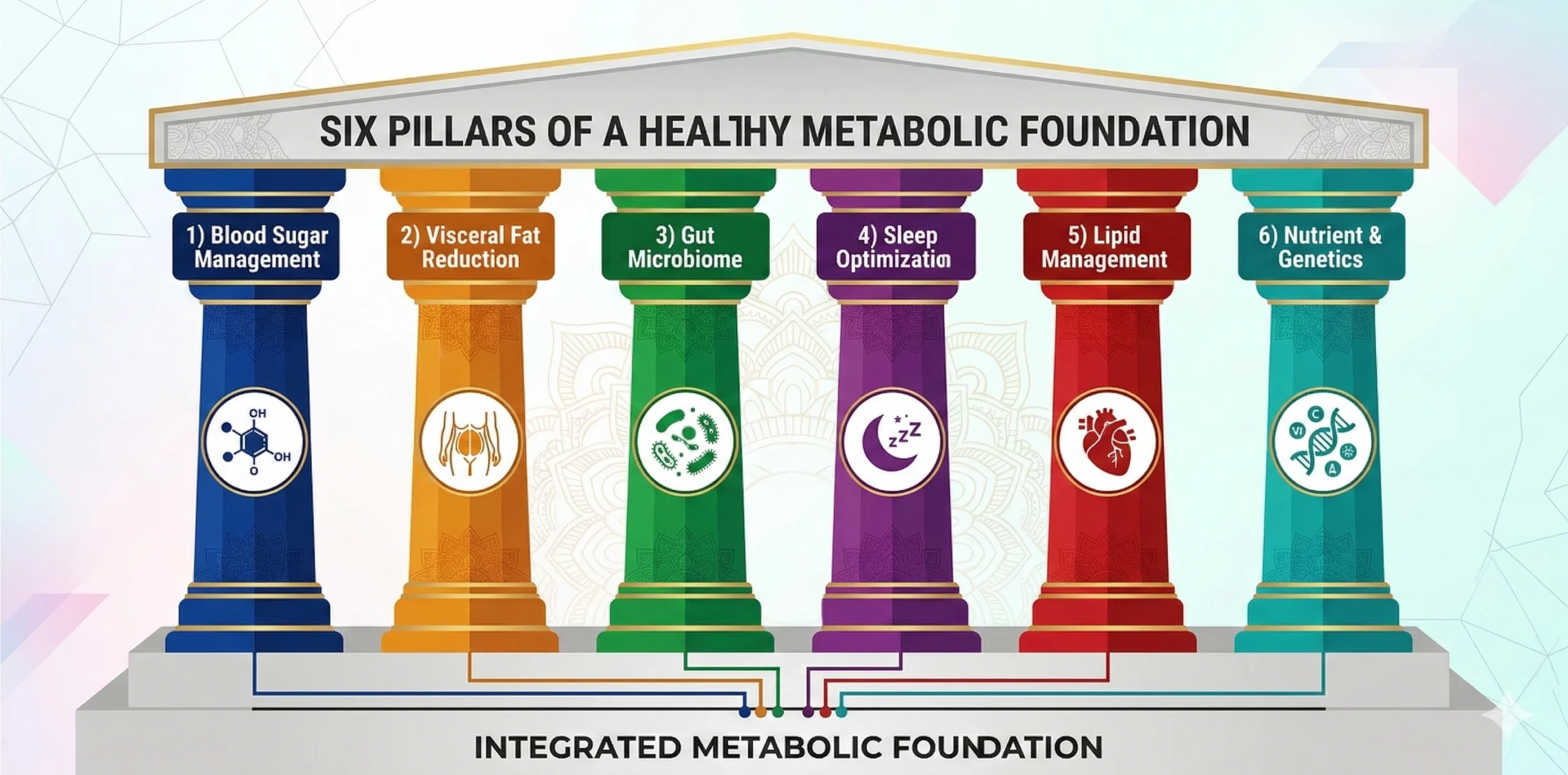
| Metabolic Pillar | Focus Area | Description |
|---|---|---|
| Pillar 1 | Blood Sugar and Carbohydrate Management | The first pillar is blood sugar and carbohydrate management. Learning how your body responds to carbohydrates is essential for preventing insulin resistance and stabilizing energy levels. Some people tolerate carbohydrates well, while others experience blood sugar spikes even with moderate intake. Understanding your personal carbohydrate tolerance can help you structure meals that maintain stable glucose levels and prevent energy crashes. |
| Pillar 2 | Reducing Visceral Fat | The second pillar focuses on reducing visceral fat, particularly the fat stored around abdominal organs. Unlike subcutaneous fat, visceral fat is metabolically active and strongly linked to inflammation, insulin resistance, and cardiovascular risk. Addressing this type of fat through targeted nutrition, movement, and stress management can significantly improve metabolic markers. |
| Pillar 3 | Supporting the Gut Microbiome | The third pillar involves supporting the gut microbiome. The trillions of microorganisms in your gut play a critical role in digestion, immune function, inflammation control, and metabolic signalling. When the gut microbiome is imbalanced, it can contribute to insulin resistance, chronic inflammation, and nutrient absorption problems. Improving gut health through fibre-rich foods, fermented foods, and diverse plant intake can support metabolic recovery. |
| Pillar 4 | Sleep Optimization | The fourth pillar is sleep optimization. Sleep is one of the most underestimated components of metabolic health. Poor sleep disrupts hormonal balance, increases cortisol levels, and reduces insulin sensitivity. Even a few nights of inadequate sleep can impair glucose metabolism and increase appetite-regulating hormones. Prioritizing consistent, high-quality sleep helps the body repair cells, regulate hormones, and maintain metabolic stability. |
| Pillar 5 | Lipid Management | The fifth pillar focuses on lipid management, particularly maintaining healthy triglyceride and cholesterol levels. Elevated triglycerides often signal metabolic dysfunction and insulin resistance. Improving lipid balance through nutrition, physical activity, and omega-3 intake helps reduce inflammation and protect cardiovascular health. |
| Pillar 6 | Nutrient Deficiencies and Genetic Predispositions | The final pillar addresses nutrient deficiencies and genetic predispositions. Micronutrient gaps such as low vitamin D, B12, magnesium, or omega-3 levels, it can impair energy metabolism and hormonal balance. Additionally, genetic variations can influence how the body processes fats, carbohydrates, and nutrients. Understanding these root causes allows for a more personalized approach to metabolic health restoration rather than relying on generalized health advice. |
When these six pillars are addressed together, metabolic health becomes far easier to restore and maintain over the long term.
Metabolic Age vs Chronological Age
Your chronological age is simply the number of years you've been alive. But your metabolic age tells a very different story, it reflects how well your body is functioning internally. Metabolic age is influenced by factors such as body composition, blood sugar control, lipid levels, inflammation, and mitochondrial efficiency. In other words, it measures whether your metabolism is functioning like someone younger, older, or the same as your actual age.
Why does this matter? Because metabolic age is closely linked to long-term health and disease risk. Someone who is 35 years old chronologically could have the metabolic profile of a 50-year-old if their blood sugar regulation, lipid levels, and inflammation are poorly controlled. On the other hand, a person in their 50s with strong metabolic markers may have a metabolic age closer to their 30s. This difference often determines how much energy you feel, how efficiently you burn fat, and your risk of developing chronic diseases.
One of the major drivers behind accelerated metabolic aging is oxidative stress. When the body is exposed to chronic inflammation, unstable blood sugar, poor nutrition, or environmental stressors, it produces excess free radicals that damage cells over time. This cellular damage affects mitochondria, the energy-producing units of the body and gradually speeds up biological aging. Over time, this process contributes to insulin resistance, reduced metabolic flexibility, and higher risk for metabolic disorders.
The encouraging news is that metabolic age is not fixed. Unlike chronological age, it can improve with the right lifestyle changes. Stabilizing blood sugar, reducing visceral fat, improving sleep quality, managing stress, supporting gut health, and correcting nutrient deficiencies all play a role in slowing metabolic aging. Regular physical activity, especially strength training and moderate-intensity cardio, it also improves mitochondrial function and helps the body use energy more efficiently.
By focusing on these lifestyle factors, it's possible not only to protect metabolic health but also to gradually reduce metabolic age and improve overall biological resilience.
The Role of DNA in Metabolic Health
Have you ever noticed this? Two people start the same diet, follow the same workout plan, and live almost identical lifestyles. Yet the results are completely different. One person loses weight easily, has stable energy, and improved blood sugar levels. The other struggles with fatigue, sugar cravings, stubborn belly fat, or rising cholesterol. Most people assume the difference is discipline or willpower. But science tells us something else. A large part of the answer lies in your DNA.
Your genes influence how your body processes carbohydrates, metabolises fats, responds to nutrients, and even how efficiently you burn calories. This is why nutrition that works beautifully for one person may completely fail for another.
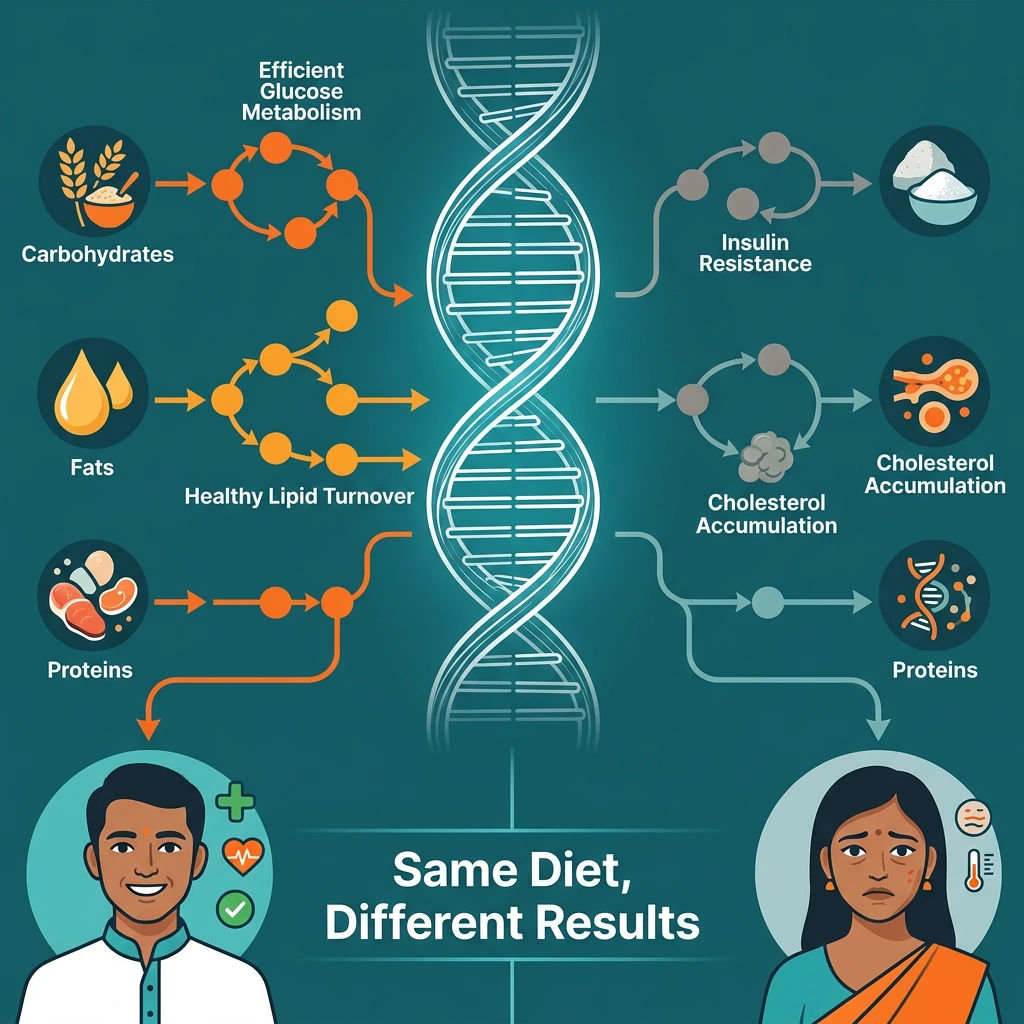
Why Two People on the Same Diet Get Different Results
Your metabolism is not only shaped by lifestyle — it is also guided by genetic instructions.
These instructions influence several metabolic processes:
- How efficiently you break down carbohydrates
- How your body handles fats and cholesterol
- How sensitive your cells are to insulin
- How your body responds to omega-3 fatty acids
- How easily your body stores or burns fat
For example, someone may thrive on a higher carbohydrate diet, while another person may experience blood sugar spikes and weight gain on the exact same foods. Similarly, some people metabolise fats efficiently, while others may develop high triglycerides or cholesterol even with moderate fat intake. This is not random — it is often genetically influenced.
Key Gene Variants That Influence Metabolic Health
Research in nutrigenomics has identified several gene variants that play a major role in how we process nutrients.
1. Genes Affecting Carbohydrate Tolerance: Certain gene variants influence how the body handles glucose and insulin. People with these variants may experience:
- Faster blood sugar spikes after carbohydrate-rich meals
- Higher risk of insulin resistance
- Greater tendency toward weight gain on high-carb diets
For such individuals, controlling refined carbohydrates and sugar intake can significantly improve metabolic health.
2. Genes Involved in Fat Metabolism: Genes also regulate how efficiently the body processes fats. Some people have variants that make them more sensitive to saturated fats, meaning their cholesterol levels may rise more easily when consuming foods like butter, processed meats, or fried foods. Others metabolise fats efficiently and may actually do well on moderate or higher healthy fat diets. This is why blanket advice like "low fat for everyone" or "high fat for everyone" often fails.
3. Genes Influencing Omega-3 Response: Omega-3 fatty acids are well known for supporting heart health, brain function, and inflammation control. However, not everyone converts or utilises omega-3 fats equally well. Certain gene variants affect how efficiently the body converts plant-based omega-3 (like ALA from flaxseeds or walnuts) into the more active forms EPA and DHA.
For these individuals, relying solely on plant sources may not be sufficient, and direct sources like fatty fish or supplements may be more beneficial.
How Nutrigenomics Personalises Metabolic Health
This is where nutrigenomics comes in. Nutrigenomics studies how genes interact with nutrients, helping us understand why different bodies respond differently to the same diet. Instead of following generalised diet trends, nutrigenomics allows nutrition to become personalised and precise.
By analysing specific gene markers, it becomes possible to:
- Understand your carbohydrate tolerance
- Identify the type of fats best suited for your metabolism
- Optimise omega-3 intake
- Improve blood sugar regulation
- Support weight management more effectively
In other words, it helps answer a powerful question: What does your body need to function at its best? As research in this field continues to grow, nutrigenomics is slowly shifting the conversation around health from "one diet fits all" to "the right diet for your biology." For a deeper understanding of how your genes influence nutrition and health, you can explore more in our DNA and nutrigenomics blog.
Metabolic Health Diet
What you eat every day plays one of the biggest roles in determining your metabolic health. A metabolic health diet focuses on reducing inflammation, stabilizing blood sugar, supporting gut bacteria, and improving lipid balance. The goal is not extreme restriction but building a sustainable way of eating that keeps your metabolism functioning efficiently.
For Indian diets, emphasizing anti-inflammatory whole foods is a great starting point. This includes vegetables like spinach, gourds, broccoli, and carrots; seasonal fruits; whole grains such as millets and brown rice; and healthy fats from nuts, seeds, and cold-pressed oils. Traditional ingredients like turmeric, ginger, garlic, and cinnamon also contain natural anti-inflammatory compounds that support metabolic function. Minimizing ultra-processed foods, refined sugars, and excessive fried foods can significantly reduce chronic inflammation and insulin resistance.
Certain foods also play an important role in supporting gut health and stabilizing blood sugar levels. Fiber-rich foods such as legumes, lentils, oats, vegetables, and seeds help slow glucose absorption and feed beneficial gut bacteria. Fermented foods like curd, buttermilk, and homemade pickles can help maintain a diverse microbiome, which is closely linked to metabolic regulation and immune balance.
Another important aspect of metabolic nutrition is lipid management, particularly maintaining healthy triglyceride and cholesterol levels. Nutrients such as plant sterols, found in nuts, seeds, and certain vegetable oils, help reduce cholesterol absorption in the body. Omega-3 fatty acids, commonly found in fatty fish, flaxseeds, and walnuts, help lower inflammation and improve lipid balance. Including these nutrients regularly in meals can support heart health while also improving overall metabolic function.
When these dietary principles are followed consistently, food becomes one of the most powerful tools for restoring metabolic health and preventing long-term chronic disease.
Final Takeaway
Metabolic health is not defined by a single lab result or number on the weighing scale. It's a system of interconnected processes that includes blood sugar control, lipid balance, inflammation levels, gut health, hormone regulation, and energy metabolism. When even one of these systems starts to drift out of balance, it can gradually affect the others. That's why focusing on just one marker like weight, cholesterol, or HbA1c, often misses the bigger picture. True metabolic health comes from understanding how all these factors work together and addressing the root causes behind dysfunction.
The encouraging part is that metabolic health is highly responsive to the right interventions. With the right nutrition, movement, sleep, stress management, and targeted nutrient support, the body has an incredible ability to restore balance and improve metabolic efficiency over time.
If you want to understand your metabolism at a deeper level, the Unlock.fit consultation is designed to help you do exactly that. Through a combination of DNA insights, advanced blood markers, and lifestyle analysis, the program helps identify your unique metabolic risks and provides a personalized roadmap to improve your health from the inside out.
External References:
- A significant percentage of adults may be metabolically unhealthy despite appearing lean. https://pmc.ncbi.nlm.nih.gov/articles/PMC10989317/
- Chronic inflammation is linked to increased risk of metabolic disorders. https://pmc.ncbi.nlm.nih.gov/articles/PMC7919414/
- Nutrient deficiencies can significantly impact metabolic health. https://www.nature.com/articles/s41591-025-03949-4
- Lifestyle changes can lead to improvements in metabolic markers within weeks. https://www.ncbi.nlm.nih.gov/books/NBK587401/
Frequently Asked Questions
Can metabolic health be reversed naturally?
In many cases, yes. Early metabolic dysfunction—such as insulin resistance, high triglycerides, or abdominal fat—can be reversed naturally. Nutrition, regular physical activity, better sleep, and stress management can significantly improve blood sugar control, lipid levels, and inflammation markers over time.
What is the fastest way to improve metabolic health?
The most effective approach is addressing multiple lifestyle factors at once. Stabilizing blood sugar through balanced meals, increasing daily movement, improving sleep quality, and reducing ultra-processed foods can lead to noticeable metabolic improvements within a few weeks to months.
Is metabolic syndrome the same as diabetes?
No. Metabolic syndrome is a cluster of risk factors such as high blood sugar, elevated triglycerides, low HDL cholesterol, high blood pressure, and increased waist circumference that increase the risk of developing conditions like type 2 diabetes and heart disease. Diabetes is a specific disease that can develop if metabolic dysfunction progresses.
Can DNA testing help improve metabolic health?
Yes, genetic insights can help explain why some people develop metabolic issues even with similar lifestyles. DNA testing can reveal variations related to insulin sensitivity, lipid metabolism, inflammation, and nutrient processing. Understanding these predispositions allows for more personalized nutrition and lifestyle strategies.
How long does it take to improve metabolic health?
The timeline varies depending on the severity of metabolic dysfunction and how consistently lifestyle changes are implemented. Some markers, like blood sugar and energy levels, may improve within a few weeks, while changes in lipid levels, body composition, and inflammation can take several months of sustained effort.
Book Your Free Consultation
If you want a diet plan tailored to your lifestyle and food preference, you can start with a free consultation.
Book Your Free Consultation
Share this article
Nupur Sharma
Nupur Sharma is a Sports Nutritionist. She has a scientific approach towards nutrition. She passionately unfolds latent aspects linking nutritional science and sports performance so that athletes and fitness enthusiasts can achieve their highest potential. She holds a Master’s degree in Sports Nutrition and Bachelor’s degree in Food, Nutrition and Dietetics.