Indian Diet Chart for Diabetic Patients: Complete Guide for Blood Sugar Control

Diabetes is everywhere in India now. Over 100 million Indians are living with it, and if you're reading this, chances are you or someone you love is managing blood sugar levels every single day.
Here's what most people get wrong: they think diabetes management is all about medication. But here's the truth – what you eat matters more than you probably realize. Your breakfast, that mid-morning snack, your dinner timing – all of it directly affects whether your blood sugar stays stable or goes on a roller coaster ride.
The problem? Most diabetes diet advice out there is completely disconnected from how Indians actually eat. You'll find plans recommending quinoa salads and kale smoothies, when what you really want to know is: can I eat my dal-chawal? What about my morning chai? Is paneer okay?
This blog on: Diet chart for Diabetic Patient is different. We're talking real Indian food – the kind you actually cook at home. No fancy ingredients. No complicated recipes. Just practical advice that works with your lifestyle, your budget, and your taste buds.
Why Your Diet Actually Matters More Than You Think
Look, I get it. When you're diagnosed with diabetes, everyone starts telling you what you can't eat. Can't have sugar. Can't eat rice. Can't enjoy festivals. It's exhausting.
But here's what's actually happening in your body: every time you eat, your blood sugar levels change. That's normal – it happens to everyone. The difference with diabetes is that your body struggles to bring those levels back down. This often happens because of insulin resistance, where your cells stop responding properly to insulin.
When you get your diet right, here's what improves:
Your blood sugar stops doing those crazy spikes and crashes. You know that feeling – eating something and then feeling shaky an hour later? That stops.
Your body starts responding better to insulin, whether it's insulin you're taking or insulin your pancreas is still making. This is huge because it means you might need less medication over time (always talk to your doctor before changing doses, though).
You'll probably lose some weight without really trying. Weight loss is especially important if you have fatty liver disease, which commonly occurs alongside diabetes. And I'm not talking about those dramatic transformations you see on Instagram. Just steady, sustainable weight loss that actually helps your diabetes.
Your HbA1c – that three-month average blood sugar reading – comes down. Many people see their HbA1c drop by 1-2 percentage points within three months of cleaning up their diet. That's the difference between "poorly controlled" and "well managed."
You lower your risk of the scary complications – kidney problems, eye damage, nerve issues, heart disease. This is the real reason to take diet seriously.
A good diabetes diet isn't about deprivation. It's about eating in a way that keeps your blood sugar steady, gives you energy throughout the day, and lets you actually enjoy your food. Understanding your overall metabolic health – not just blood sugar – is key to long-term diabetes management. It's possible. You just need the right information.
Understanding How Indian Foods Affect Your Blood Sugar
Before we jump into meal plans, you need to understand one concept: the Glycemic Index, or GI. Don't worry, this isn't complicated.
The GI is basically a ranking of how quickly a food makes your blood sugar go up. High GI foods cause a rapid spike. Low GI foods release sugar slowly and steadily.
Here's the simple version:
- Low GI (55 or below): These are your friends. Eat them freely.
- Medium GI (56-69): Okay in moderation, especially with protein and vegetables.
- High GI (70+): These spike your blood sugar fast. Limit them.
Let's talk about the foods you actually eat:

| Low GI Foods (Good for Diabetics) | GI Range | Why It's Good |
|---|---|---|
| Whole moong dal | Low (Below 55) | One of the best protein sources, keeps blood sugar stable |
| Chickpeas/chana | Low (Below 55) | Great for blood sugar control, high fiber and protein |
| Rajma/kidney beans | Low (Below 55) | High protein, low GI, very filling |
| Whole wheat roti | Low-Medium (45-50) | Much better than white bread, good fiber content |
| Brown rice | Low-Medium (50-55) | Better choice than white rice, has fiber and nutrients |
| Most vegetables (spinach, beans, cauliflower, etc.) | Very Low (15-30) | Eat unlimited amounts, high fiber, minimal sugar impact |
| Apples, guavas | Low (35-40) | Your go-to fruits, natural sugar with fiber |
| Curd/yogurt | Low (35-40) | Excellent probiotic, helps with gut health and insulin sensitivity |
| High GI Foods (Limit These) | GI Range | Why Be Careful |
|---|---|---|
| White rice (Sona Masuri, Ponni) | High (70-77) | Rapid blood sugar spike, keep portions very small |
| White bread, maida products | High (75+) | Spikes blood sugar quickly, low nutritional value |
| Potato (boiled) | High (78+) | Higher than expected, limit portions significantly |
| Cornflakes, packaged cereals | High (80+) | Surprisingly high GI, avoid for breakfast |
| Traditional sweets (gulab jamun, jalebi) | Very High (85+) | Pure sugar, causes severe spikes, avoid completely |
Here's the thing about rice: I know what you're thinking – "but I've eaten rice my whole life!" And I'm not telling you to give it up completely. Here's what actually works:
Switch to brown rice or hand-pounded rice when possible. The GI is lower (around 50-55). If you must have white rice, keep portions small (half to two-thirds cup cooked) and always eat it with dal and lots of vegetables. The protein and fiber slow down the sugar absorption. Consider having rice only once a day instead of twice.
Your Practical Indian Diet Chart
Alright, let's get to what you actually came here for – what to eat, when to eat it, and how much.
These aren't rigid rules. They're templates. Adjust based on your appetite, your schedule, and what you actually enjoy eating. The best diet is one you'll actually stick to.
Daily calorie targets (roughly):
- If you're mostly sitting at a desk: 1,500-1,800 calories
- If you're moderately active: 1,800-2,200 calories
- If you're very active: 2,200-2,500 calories
How your plate should look:
- 40-45% carbs (yes, you can have carbs – just the right ones)
- 25-30% protein (this is more important than most people realize)
- 25-30% healthy fats

Complete Day's Meal Plan at a Glance
| Meal Time | What to Eat | Protein Target | Key Points |
|---|---|---|---|
| 6:00-7:00 AM (On wake-up) |
Methi water OR Apple cider vinegar water OR Cinnamon tea OR Moringa powder | - | Helps with blood sugar control, drink 30 min before breakfast |
| 8:00-9:00 AM (Breakfast) |
Vegetable oats + curd OR 2 multigrain rotis + sabzi + curd OR Besan chilla + chutney OR 2 idlis + sambar + paneer | 15-20g | Never skip breakfast, include protein to stay full till lunch |
| 11:00-11:30 AM (Mid-morning snack) |
1 fruit + nuts OR Veggie sticks + hummus OR Roasted chana OR Sprouts salad OR Curd + seeds | 5-10g | Prevents 4-hour gap, whole fruits only (never juice) |
| 1:00-2:00 PM (Lunch - biggest meal) |
1-2 rotis/½-⅔ cup brown rice + 1 cup dal/rajma/paneer + 1.5-2 cups vegetables + Large salad + 1 cup curd | 20-25g | Follow plate method: 50% veggies, 25% protein, 25% carbs |
| 4:30-5:00 PM (Evening snack) |
Roasted makhana OR Vegetable soup OR Sprouts chaat OR 2 dhoklas OR Boiled egg/grilled paneer | 5-10g | Prevents dinner overeating, avoid biscuits and fried snacks |
| 7:00-8:00 PM (Dinner - lighter) |
1 roti (optional) + Large bowl vegetable sabzi + 100g paneer/tofu/egg + 1 cup curd OR Soup + vegetables | 15-20g | Eat 2-3 hours before sleep, keep lighter than lunch |
Total Daily Protein Target: 60-90g (for a 60kg person at 1.0-1.5g per kg body weight)
First Thing in the Morning (6:00-7:00 AM)
Before breakfast, try one of these. They genuinely help with blood sugar control:
Methi water: Soak a teaspoon of fenugreek seeds in water overnight. Drink the water first thing in the morning. Tastes bitter but many people swear by it.
Apple cider vinegar: One tablespoon in a glass of warm water. Some find it helps with blood sugar.
Cinnamon tea: Green tea with half a teaspoon of cinnamon powder. Easy and pleasant.
Moringa powder: One teaspoon in warm water. Rich in antioxidants.
Have whichever one you can actually stick to. There's no point in forcing yourself to drink something you hate every morning.
Breakfast (8:00-9:00 AM)
Never skip breakfast if you have diabetes. I know mornings are rushed, but skipping breakfast sets you up for blood sugar problems all day.
Option 1: Vegetable Oats
Half cup oats cooked with vegetables – carrots, beans, peas, whatever you have. Add a tablespoon of flaxseeds. Eat with a cup of curd. This keeps you full for hours.
Option 2: Multigrain Roti
Two small rotis made from wheat mixed with jowar, bajra, or ragi. Have them with vegetable sabzi and thick curd. Add some almonds on the side.
Option 3: Besan Chilla
Two chickpea flour pancakes loaded with onions, tomatoes, and spinach. Eat with mint chutney and curd. High protein, filling.
Option 4: South Indian (Modified)
Two small idlis with extra sambar. Skip the coconut chutney – it's high in calories. Add an egg or some paneer for protein.
Option 5: Moong Dal Chilla
These are lighter than besan but just as filling. Two chillas with buttermilk and a handful of walnuts.
The key with breakfast: aim for 15-20 grams of protein. This stabilizes your blood sugar for the entire morning and stops those mid-morning cravings. If you're vegetarian and wondering how to get enough protein, check out our complete guide to protein-rich vegetarian foods available in India.
Mid-Morning Snack (11:00-11:30 AM)
Don't go more than four hours without eating. Long gaps cause blood sugar to drop and then spike when you finally eat.
Option 1: One small apple or guava with 6-8 almonds
Option 2: Cucumber and carrot sticks with two tablespoons of hummus
Option 3: Quarter cup roasted chana with green tea
Option 4: Half cup sprouts with lemon and chaat masala
Option 5: Cup of thick curd with a tablespoon of mixed seeds
About fruits: You can eat them, but choose wisely. Apples, guavas, pears, and berries are great. Go easy on mangoes, bananas (especially very ripe ones), and grapes. And please – whole fruits only. Never juice. Juicing removes all the fiber and leaves you with just sugar.
Lunch (1:00-2:00 PM)
This should be your biggest meal. Eating a proper lunch prevents evening hunger and stops you from overeating at dinner.
The template that works:
Pick one carb:
- 1-2 small multigrain rotis, OR
- Half to two-thirds cup brown rice (measured after cooking), OR
- One cup quinoa (if you're willing to try it)
Pick one protein:
- Cup of dal (any dal works)
- Cup of rajma, chole, or lobia curry
- 100g paneer curry
- Cup of soy chunks or tofu
- Two eggs (boiled, scrambled, or curry)
Vegetables (mandatory):
One and a half to two cups of cooked vegetables. Focus on fiber-rich ones like lauki, bitter gourd, spinach, beans, cauliflower.
Salad (also mandatory):
A large bowl of raw salad – cucumber, tomato, onion, carrots. Use lemon and minimal salt.
Curd or raita:
One cup. The probiotics are good for your gut and may improve insulin sensitivity through the gut-hormone connection.
Here's the plate method I want you to remember:
Half your plate should be vegetables (cooked and raw). A quarter should be protein (dal or paneer). A quarter should be carbs (roti or rice). This automatically controls portions without you having to measure everything obsessively.
Some lunch combinations that work:
Two bajra rotis + moong dal + lauki sabzi + salad + curd
One roti + rajma curry (extra dal) + palak + salad + raita
Two-thirds cup brown rice + sambar (make it thick with dal) + beans curry + cucumber raita
Evening Snack (4:30-5:00 PM)
This is crucial. The evening snack prevents dinner overeating and keeps your blood sugar stable during that long gap between lunch and dinner.
Option 1: Cup of roasted makhana (foxnuts) with minimal salt – surprisingly filling
Option 2: Bowl of homemade vegetable soup (no cornflour for thickening)
Option 3: Three-quarter cup sprouts with onion, tomato, and lemon. Skip the potato sev.
Option 4: Two small steamed dhoklas with green chutney
Option 5: One boiled egg or 50g grilled paneer with veggie sticks
What to absolutely avoid:
Biscuits (yes, even "digestive" and "sugar-free" ones – they're still mostly refined flour). Namkeen and mixtures. Samosas and pakoras. Bread with jam. Chips. Bakery items.
I know these are convenient. But they mess with your blood sugar in ways that aren't worth it.
Dinner (7:00-8:00 PM)
Eat dinner at least 2-3 hours before you sleep. Late dinners worsen your fasting blood sugar the next morning.
Keep dinner lighter than lunch. Your insulin sensitivity is naturally lower at night, so carbs have more impact.
Option 1: Vegetable-Heavy Dinner
One roti (or skip it entirely) with a large bowl of mixed vegetable sabzi and 100g paneer or tofu. Cup of curd.
Option 2: Soup + Sabzi
Bowl of vegetable soup, one and a half cups of sautéed vegetables, an egg or some paneer, small salad.
Option 3: Dal-Based
One small roti, cup of dal, cup of vegetable curry, cucumber raita.
Option 4: South Indian Light
Two idlis or one dosa (no potato filling), one and a half cups sambar, tiny bit of coconut chutney.
Option 5: Khichdi
Cup of moong dal khichdi with vegetable curry on the side and curd. Comfort food that's actually good for you.
If you're hungry after dinner, have warm milk with turmeric (no sugar) or herbal tea. Don't eat carbs or sweets before bed.
Foods You Can Eat Freely
These have minimal impact on blood sugar. Eat as much as you want:
Vegetables: Spinach, methi, bottle gourd, bitter gourd, brinjal, okra, cauliflower, cabbage, mushrooms, tomatoes, cucumber. Basically, all the green vegetables your mom told you to eat.
Salad vegetables: Lettuce, cucumber, tomato, onion, bell peppers, sprouts
Beverages: Green tea, black coffee (unsweetened), lemon water, buttermilk (unsweetened)
Foods You Need to Measure
These are healthy, but portions matter:
Grains: Half to two-thirds cup brown rice (cooked), two small rotis, half cup millets, half cup quinoa, half cup oats
Proteins: Cup of dal, 100g paneer, 1-2 cups curd, 1-2 eggs
Nuts: 8-10 almonds, 4-5 walnuts, 1-2 tablespoons of seeds
Fruits: One small apple, guava, or pear; one cup berries; half cup papaya
Foods to Avoid (Or Severely Limit)
Sugars and sweets: All of it – white sugar, jaggery, honey, gulab jamun, jalebi, barfi. If you're going to have a sweet, make it a special occasion, not a daily thing.
Refined grains: White bread, maida products (naan, pizza, pasta), biscuits, cakes, pastries
Sweetened drinks: Soft drinks, packaged fruit juices, sweetened tea and coffee, energy drinks
Deep-fried foods: Samosa, pakora, puri, bhatura, chips
High-starch vegetables: Go very easy on potatoes. If you must have them, boil them and eat with lots of vegetables.
Packaged and processed foods: Instant noodles, frozen meals, packaged snacks
Want a Personalized Diabetes Diet Plan?
Generic plans don't work for everyone. Take our quiz to get insights tailored to YOUR body and metabolism.
Discover Your Metabolic Profile→Common Mistakes People Make (And How to Fix Them)
Mistake #1: Skipping meals to control blood sugar
This backfires. You end up with blood sugar fluctuations and then overeat later. Eat three meals and one to two snacks daily. Space meals 3-4 hours apart.
Mistake #2: Cutting out all carbs
Your brain needs glucose. Going zero-carb causes fatigue and isn't sustainable. Eat complex carbs in controlled portions.
Mistake #3: Drinking fruit juice instead of eating fruit
Juicing removes fiber. You end up drinking the sugar of three oranges with none of the fiber to slow absorption. Always eat whole fruits.
Mistake #4: Trusting "sugar-free" labels
Sugar-free biscuits still have refined flour. They often have more calories than regular versions. Check total carbohydrates, not just sugar.
Mistake #5: Having large dinners late at night
Your insulin sensitivity is lowest at night. Eat dinner by 7:30-8 PM. Keep it lighter than lunch.
Mistake #6: Not watching portion sizes
Even healthy foods affect blood sugar in large quantities. Use the plate method. Measure your grains and dal portions initially until you get a feel for the right amount.
Mistake #7: Only focusing on diet without exercise
Diet alone has limits. Walk 30-45 minutes daily. Even a 10-minute walk after meals helps significantly.
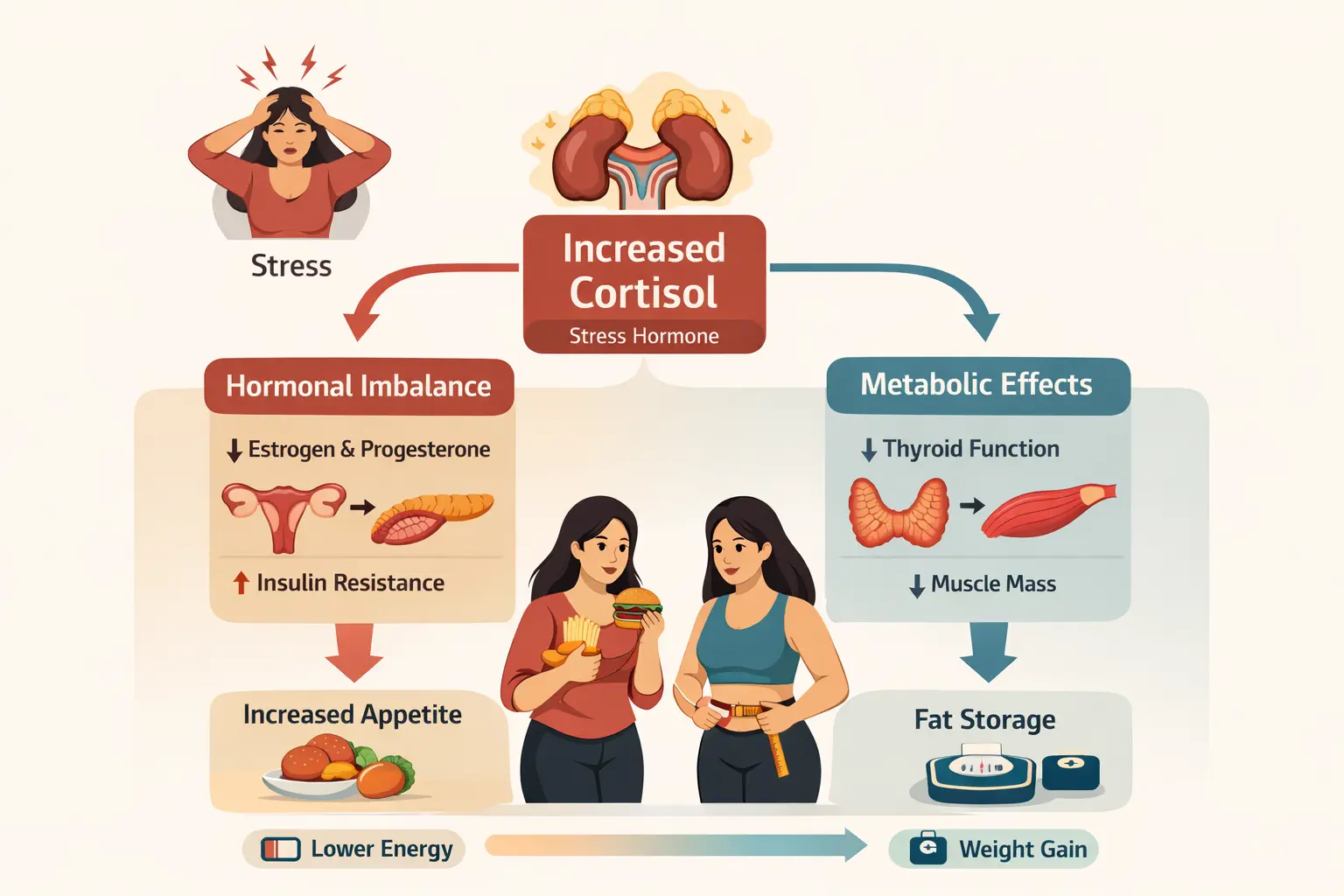
Mistake #8: Not managing stress
High cortisol from chronic stress worsens insulin resistance and makes blood sugar harder to control. Stress management isn't optional for diabetics – it's essential.
The Protein Strategy Most People Miss
Here's something most diabetes diet plans don't emphasize enough: when you eat protein matters just as much as how much you eat.
Spreading protein evenly across the day improves blood sugar control better than eating most of it in one meal.
Why this matters:
Protein slows down how quickly you absorb carbs. It reduces those post-meal blood sugar spikes. It keeps you full between meals, preventing snacking on junk. It helps preserve muscle mass, which is crucial for insulin sensitivity.
Aim for this protein distribution:
- Breakfast: 15-20g protein
- Lunch: 20-25g protein
- Dinner: 15-20g protein
- Snacks: 5-10g protein
Total daily protein: Around 1.0-1.5 grams per kilogram of your body weight. If you're trying to lose weight, you might go up to 1.5-2.0 grams per kg. If you have kidney disease, talk to your doctor – you might need to stay around 0.8 grams per kg.
For a 60kg person, that's 60-90 grams of protein daily. That's significantly more than what most Indians typically eat, and it makes a real difference.
Can Diet Alone Control Your Diabetes?
This is what everyone wants to know.
The honest answer depends on where you are in your diabetes journey:
If you're in the prediabetes stage or caught it very early: Yes, many people can control blood sugar completely with diet and lifestyle changes. It takes consistency, but it's definitely possible.
If you've had diabetes for a while: Diet will help tremendously, but you might still need medication. The good news? Many people reduce their medication doses over time with good diet control. Some go from three medications to one. Some reduce from high doses to low doses.
If you have Type 1 diabetes: Diet helps with stability and reduces how much insulin you need, but you'll always need insulin. Better diet just means more predictable insulin dosing and fewer complications.
If you've had diabetes for 10+ years: Diet is crucial for preventing complications, but it rarely eliminates the need for medication. The goal is optimal control with minimum medication.
Important: Never stop or reduce medications on your own. Any changes should happen under medical supervision with regular blood sugar monitoring. The goal isn't to eliminate medicine at all costs – it's to achieve good control (HbA1c under 7%) with the least medication needed.
Why One Diet Doesn't Work for Everyone
You know how your friend follows some diet and their diabetes improves dramatically, but you try the same thing and nothing happens?
That's because diabetes is incredibly individual. What works for someone else might not work for you.
Here's what varies from person to person:
Blood sugar patterns: Some people have high fasting sugar but normal levels after meals. Others are the opposite. Each pattern needs a different approach.
Medications: If you're on metformin, you can probably handle more carbs than someone on insulin. If you're on sulfonylureas, you need to be careful about meal timing to avoid hypoglycemia.
Weight and body composition: Someone who's overweight needs fewer calories. Someone at normal weight needs to focus on food quality, not quantity. Muscle mass affects insulin sensitivity significantly.
Age and activity: A 30-year-old needs more calories than a 65-year-old. Sedentary versus active makes a huge difference.
Other health issues: High triglycerides? You need lower carbs. High LDL cholesterol? Limit saturated fats. Low HDL? Focus on healthy fats. Kidney problems? Protein needs to be monitored carefully.
This is why personalized plans based on your actual blood reports, medications, lifestyle, and food preferences work better than following a generic chart from the internet. Improving insulin sensitivity is one of the core markers of better metabolic health and affects everything from weight management to hormone balance.
What to Actually Track
Don't obsess over your blood sugar readings every hour. But do track these regularly:
Fasting blood sugar: Target 80-110 mg/dL. Check every morning before eating.
Post-meal blood sugar: Target less than 140 mg/dL (two hours after eating). Check two hours after breakfast, lunch, or dinner.
HbA1c: Target below 7% (below 6.5% is excellent). Check every three months. This shows your three-month average blood sugar. Your HbA1c and other metabolic markers determine your metabolic age, which can be higher or lower than your actual age depending on your health.
Weight: Weekly is enough.
Waist circumference: More important than weight for diabetics.
Blood pressure: Should be below 130/80.
Lipid profile: Check every six months.
Kidney function tests: Once a year.
Eye check-up: Once a year.
Understanding what your lab results actually mean helps you make informed decisions about your diabetes management.
Ready to Take Control of Your Diabetes?
Get personalized insights based on YOUR unique metabolic profile. Free 2-minute assessment.
Start Your Assessment →Frequently Asked Questions
Q1: What is the best diet chart for a diabetic patient in India? +
There's no single "best" diet because everyone's different. But a good Indian diabetic diet includes plenty of high-fiber vegetables (unlimited), adequate protein (1.0-1.5g per kg body weight from dal, paneer, eggs, or soy), healthy fats from nuts and mustard oil, and controlled portions of low glycemic index carbs like brown rice or whole wheat rotis. The key is portion control of carbs combined with protein at every meal to slow sugar absorption.
Q2: Can a diabetic patient eat rice daily? +
Yes, but choose wisely. Brown rice, hand-pounded rice, or red rice (half to two-thirds cup cooked) can be included daily when paired with dal and plenty of vegetables. This combination significantly lowers the impact on blood sugar compared to eating white rice alone. However, limit polished white rice to 2-3 times weekly in very small portions because of its high glycemic index.
Q3: Which foods should a sugar patient completely avoid? +
Completely avoid: refined sugar and traditional sweets (gulab jamun, jalebi), sweetened beverages (soft drinks, packaged juices), deep-fried foods (samosa, pakora), refined flour products (maida, white bread, bakery items), and excessive white rice or potato. These cause rapid blood sugar spikes and provide little nutrition.
Q4: How many meals should a diabetic patient eat daily? +
Three balanced main meals plus one to two healthy snacks, spacing meals 3-4 hours apart. Never skip meals, especially breakfast. This eating pattern maintains stable blood sugar throughout the day and prevents the extreme hunger that leads to overeating.
Q5: Why does the same diet work differently for different diabetic patients? +
Individual response varies based on your specific blood sugar pattern (fasting versus post-meal issues), medications (metformin users versus insulin users need different approaches), HbA1c levels, weight, activity level, age, other conditions like PCOS or thyroid problems, cholesterol levels, kidney function, and genetic factors. This is why personalized plans based on your complete blood work deliver better results than generic diet charts.
Q6: Is intermittent fasting safe for diabetic patients? +
It can be beneficial for Type 2 diabetics not on insulin or sulfonylureas, but requires medical supervision. A gentle 12-14 hour overnight fast (dinner by 8 PM, breakfast by 10 AM) is generally safe. However, longer fasts can cause dangerous blood sugar fluctuations, especially if you're on certain medications. Never try intermittent fasting without consulting your doctor and adjusting medications accordingly. For insulin users, fasting is generally not recommended.
Your Next Steps
Managing diabetes through diet isn't about eating bland, boring food or giving up everything you enjoy. It's about understanding how your body responds to different foods and making strategic choices that keep your blood sugar stable.
Start here:
- Don't skip meals, especially breakfast
- Control portions of carbs; don't eliminate them
- Include protein at every meal – 15-20g minimum
- Fill half your plate with vegetables at lunch and dinner
- Choose low GI foods – dal, vegetables, whole grains
- Walk after meals – even 10 minutes helps
- Monitor regularly – blood sugar, HbA1c every three months
- Consider personalized guidance if generic plans aren't working
Start with small changes. Swap white rice for brown rice a few times a week. Add a 10-minute walk after dinner. Increase your vegetable portions. These small steps add up to major improvements over 3-6 months.
Your diabetes journey is unique to you. What matters is finding an approach you can actually stick to long-term – not some extreme diet you'll quit after two weeks.
You've got this. One meal at a time.
Need a Personalized Diabetes Diet Plan?
While this guide provides a solid foundation, every diabetic patient responds differently to foods based on their unique metabolic profile, medications, lifestyle, and health conditions.
Generic diet charts can only take you so far.
A personalized nutrition plan considers:
- Your current HbA1c, fasting sugar, and post-meal blood sugar patterns
- Your medications and their impact on diet requirements
- Your weight, activity level, and body composition
- Other health conditions (PCOS, thyroid, high cholesterol, fatty liver)
- Your food preferences, cooking habits, and family situation
- Your work schedule and lifestyle constraints
Our clinical nutritionists specialize in creating customized diabetes diet plans for Indian patients that actually work with your real life – not against it.
Book Your Free Consultation Today
Get a personalized diabetes diet plan based on your blood reports, medications, and lifestyle. Our nutrition experts will help you achieve better blood sugar control in a way that actually fits your life.
✓ One-on-one consultation with certified nutritionist
✓ Blood report analysis (HbA1c, fasting sugar, lipid profile)
✓ Customized meal plan with portion sizes
✓ Indian recipes you'll actually enjoy
✓ Ongoing support to reduce medications safely
Limited slots available. Takes 60 seconds to schedule.
Don't let generic advice hold you back. Get a plan that's designed specifically for YOUR body and YOUR goals.
Share this article
Nihala Ibrahim
Nihala Ibrahim is a clinical dietitian with a scientific approach to personalized nutrition and metabolic health. She passionately bridges clinical insights with evidence-based diet strategies to help clients overcome diabetes, thyroid issues, PCOS, and weight challenges for optimal wellness. She holds Masters in clinical dietetics and nutrition science from Sri Ramachandra Institute, Chennai.